“It’s the most unnatural situation to leave your baby and go home. That’s not how it’s supposed to be. You’re supposed to leave the hospital with your baby in your arms,” says Sarah Bender Hope. Her son, Solomon, was born at 25 weeks’ gestation in 2015, just two years after her first son, Isaiah, passed away at 23 weeks old.
Bender Hope recalls her first experience with the neonatal intensive care unit team at Mission Children’s Hospital. “They administered comfort care to my first son, Isaiah. I think that meeting them and knowing that they honored the pregnancy and honored my baby and were there to make sure that he only knew peace while he was on Earth just really made me have a lot less trauma in a majorly traumatic situation.”
Her second son, Solomon, spent a total of 106 days in the NICU, and once Bender Hope regained her own health, she spent an average of nine hours a day sitting beside him.
Linda Yandell Smith, NICU nurse manager at the hospital, said via email, “More than 67 percent of the babies who come to Mission’s NICU actually stay less than 10 days. This is because of improved perinatal care to pregnant moms. Babies are able to stay inside the mom longer, and every day can count.”
Mission’s NICU cares for the tiniest patients from all over Western North Carolina in its 51-bed facility, often bringing them in by helicopter or emergency transport. Jessica Edwards, family support and outreach coordinator, says, “We serve all [17 counties] of Western North Carolina. … Sometimes we have babies that come in from Tennessee and South Carolina.”
Nicole Kintz’s daughter, Nina, was born seven weeks early and spent three weeks in the NICU. “At the time of her birth they gave a pre-diagnosis of Down syndrome, and we just had that confirmed two weeks ago,” says Kintz. “She spent three weeks in the NIC unit basically just trying to get bigger and learning how to be. That was her main thing. Babies don’t learn how to suck, swallow and breathe until 35 weeks in utero, and she was 33 weeks. So, she had to learn a skill that she wasn’t quite ready for, and that was stressful. That was the only way I was going to get her home — when she was able to feed all on her own. … We basically taught her that skill.”
Ashley English’s son, Alistair, was born at 27 weeks and spent 79 days in the NICU. English felt grateful that she lived close enough to visit her son every day during his long stay. “There were a lot of parents who could not be there every day. Either they lived too far away or they had to work, and they were waiting until the baby was discharged so that they could take maternity leave then,” says English.
What made a difference during a traumatic time to these three parents of premature infants who spent enough time inside the NICU to learn it like the back of their hands? The caring staff. “The nurses are probably some of the most compassionate, empathetic, giving people that I’ve ever met in my life. They will go above and beyond to connect with a family, to bring a family comfort, to make sure that a family has the resources that they need before they leave our hospital,” says Edwards.
“Every breakdown I had, I swear, a nurse would sit with me,” says Kintz. “The head nurse of the NIC unit caught me one day just crying, and she sat with me for an hour, held my hand. It was so beyond just medical care. I just had so many nurses sit with me and share their experience, give me their tips. You know, everyone has a tip for you, and as stressful as that could be, it was really a magical experience. I just can’t say enough about how grateful I am to those people.”
English notes that all of the nurses who work in the NICU are remarkable, but one nurse in particular, Charleen Ballard, went the extra mile to bring comfort during a traumatic time. “On my husband’s birthday, she brought him a hat that had belonged to her dad. On Mother’s Day, she left me a gift. For Alistair (when we left, my nickname for him was ‘Chicken’ because he looked like a little plucked chicken) she bought him these little soft-soled shoes that had chickens on them. She brought me earrings when I was in the hospital that had belonged to her mother, who used to own a chicken farm; they’re little chicken earrings. She brought me a copy of the book The Help. She completely became like family, and she just loved Alistair. She called him ‘Sunshine.’ She would walk up to his crib and say, ‘Hey, Sunshine.’ I just love her. She blew my mind. I just had no idea that somebody could make us feel like it was going to be all right.”
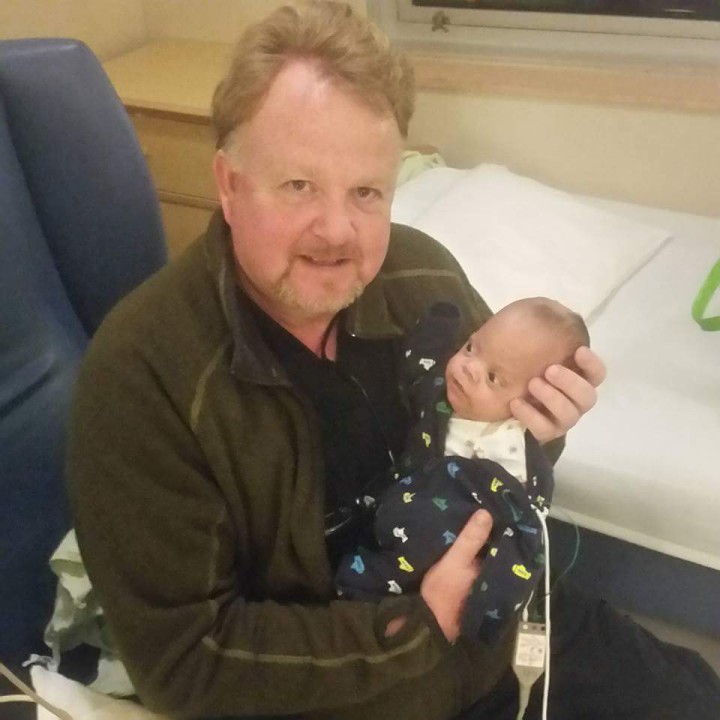
English was not the only one who had a nurse to remember. For Bender Hope, that nurse was Andy Evans. “Our primary nurse … means the world to me, ” she says. “Andy and Solomon had this little NICU dance that they did together, and Andy was a part of major incidents at the hospital with Solomon. And I felt so connected to him, and Solomon and him just had this amazing energy back and forth that was just crazy to watch. He became part of our family.”
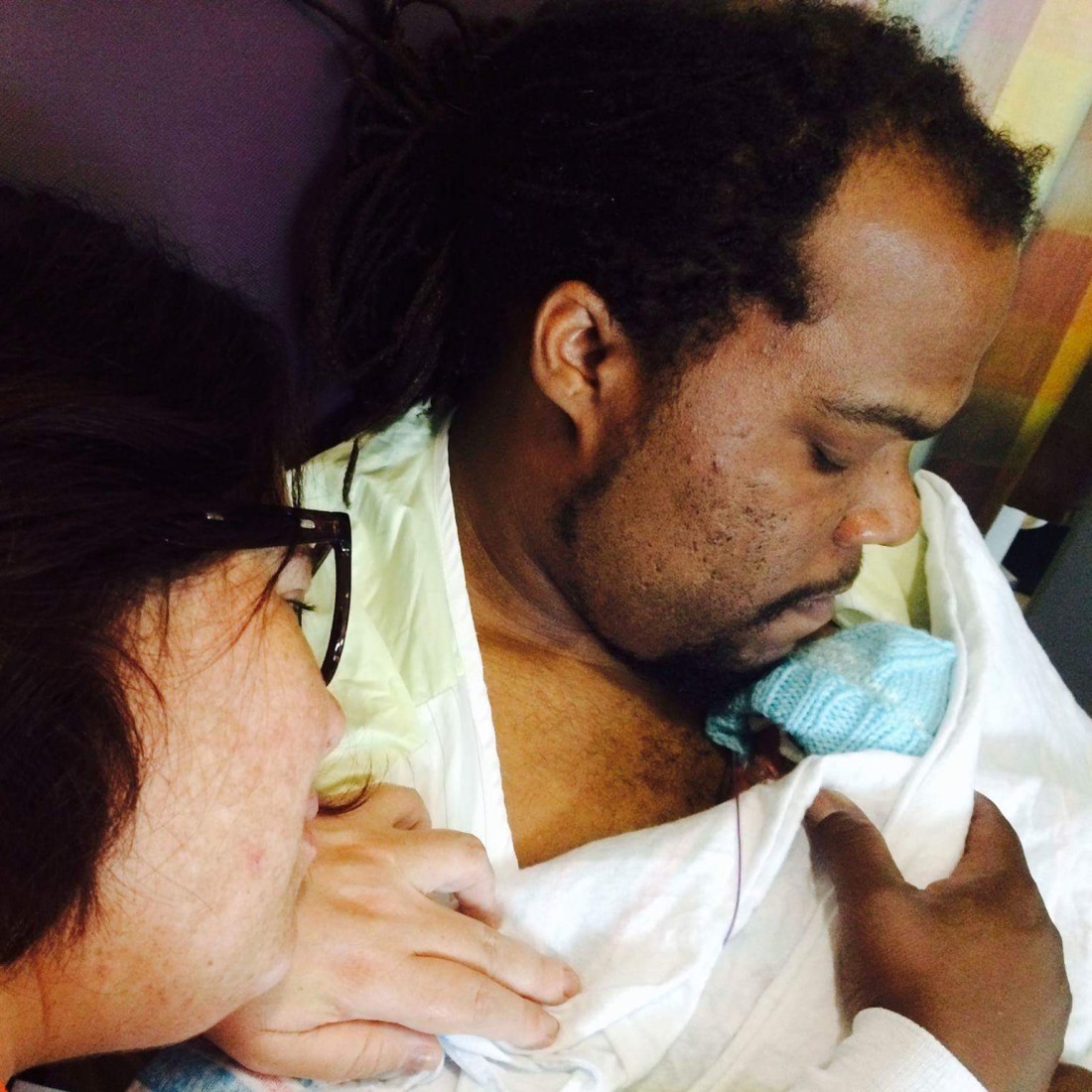
“One of my favorite things in the NICU was to do skin-to-skin. They call it ‘kangaroo care,’ and that’s really healing for the babies because they’re back on their mama’s skin, they’re hearing the heartbeat, and they can feel the love you’re sending them,” she continues. “As they get bigger, you can hold them longer because they could hold their body temperature longer, and he [Evans] would say, ‘What I always tell people is when you hold your baby, think about the dreams that you have for them, because you’re going to be excited, and they are going to feel that energy and feel that love that you have for them.’ And so, I just had these visions of Solomon as a little boy and Andy and him going fishing together, which was like funny to me because we just met this man, but he was part of this vision that I had for my son.”
Because of her experience in the NICU, Bender Hope has become part of the NICU Family Advisory Council. “We have different initiatives that we set every year to basically help make the place a little bit better for the parents to kind of give the voice of the parent to the nurses in the unit so that they can hear what works and what doesn’t work and just make it a better situation for somebody that’s sitting there with their baby at their bedside,” she explains.
Bender Hope also donates her services as a bereavement doula. “Because of Isaiah, I’ve also become a bereavement doula, which I do in the NICU and the city as well,” she says. “I think that one thing I’ve learned from my sons is: I’m not the first one to have a son that passed away, and I’m not the first one to have a micro-preemie, but unfortunately, I’m not the last one either. So, something that I was raised with was that you are a part of the community, and you give back.”


Hi Jacqui: this is a nice and heartwarming article, but out of curiosity — was it pitched to you or Mountain Xpress by Mission’s PR department? Given the hospital’s ongoing dispute with BCBSNC, a feel-good piece about the hospital’s work in caring for babies — something that nobody was actively questioning — seems very loaded.
You are, in effect, saying that the Physicians, Nurses and other staff who actually PROVIDE CARE should not be afforded any recognition for their services because you disagree with the financial or political positions taken by the hospital’s CORPORATE management.
Very “progressive”.
Maybe pull your head out of your politics for a moment and your worldview will not be so polluted?
It is the role of the “progressive” to be skeptical of suspicious timing, but to inquire respectfully into the facts before leaping to conclusions, as Luther has admirably done here. If you don’t like that, Big Al, you can find plenty of venues on the Internet that cater to an alt-approach.
I would assert that assuming an article about Mission nurses originated from corporate PR rather than from grateful families (as it turned out to be) is the very definition of leaping to conclusions.
You can visit http://www.standwithmission.com to understand more of Mission’s side of the argument. BCBS has a history of “bullying” many hospitals, large and small. You can find out more about other cases involving BCBS through a simple google search. MD Anderson of Houston, one of the largest hospitals in the country, had the same experience with BCBS. In essence our healthcare system is broken and hopefully and agreement will be reached by both parties.
Hi Luther, I am one of the parents that was featured in the article. I just came across your question and I realize that Jacqui answered your question, however, I am honestly insulted. This article was an amazing way for me and the other mothers to share our stories about the medical staff who helped saved our precious babies. There was absolutely NOTHING mentioned that was politically based re: the Mission/BCBS situation.
There are a vast amount of news articles that are written that are not addressing specific questions but community interest. The work in the NICU is often misunderstood and scary for some. This was an opportunity to share an insight as to what is a restricted area filled with precious lives. Instead of taking the chance to question the motive, how about simply reading and learning OR move on.
Hello, Luther. I can answer your question: The story was actually pitched to me by Ashley English, a parent whose baby was born extremely prematurely and spent a few months in Mission’s NICU. I interviewed Ashley for a story that ran in the Food section several weeks ago, and she mentioned numerous times during our conversation the excellent care her baby received in the NICU and the above-and-beyond kindness she and her family were shown by the staff. She suggested that a story about it might be of interest to readers, and I passed that along to our Wellness editor, Susan Foster, who gave the assignment to Jacqui Castle.
Thanks, Gina, for such a prompt and thorough response.
I wish Mission Health went “above and beyond” for their staff. My mother worked in the Mother/Baby Unit, previously the Nursery, of the hospital since she graduated from AB-Tech 38 years prior. Only a few years from retirement, she was let-go not because of her actions as a nurse, but because she was not an RN. My mother was an LPN that could work circles around and knew more, through years of experience, than the many inexperienced RNs that came long after. Instead of being valued as an asset to the team, she was dismissed. After asking for compensation for her dismissal, they offered her only $1000 severance. If given the choice, I will always choose to go ANYWHERE other than Mission Health. Though that limits my options since they have monopolized our region. Disappointing.