When Dr. Jennifer Mullendore told the Buncombe County Board of Commissioners last October that immunization exemptions for local kindergartners had jumped again, she didn’t know that at least one local child was already sick with chickenpox. Mullendore is the medical director at Buncombe County Health and Human Services.
By the end of that month, 28 children had contracted the illness, all of them at the Asheville Waldorf School. The eventual total of 37 students (all of them unimmunized) and three community members diagnosed with the virus constituted the most in the state since the varicella vaccine became available in 1995 and the immunization was required for school enrollment. According to Alice Elio, school health program manager at the Mountain Area Health Education Center, the Centers for Disease Control and Prevention considers five or more related cases of chickenpox to constitute an outbreak.
Mullendore, a family medicine physician, mother and outspoken advocate of immunization, didn’t come to the Board of Commissioners’ Oct. 2 meeting seeking additional funding or policy changes. She merely cited facts: In the 2017-18 school year, 145 children in Buncombe County — 5.7 percent of kindergarten students — received religious exemptions from one or more of the vaccinations required within 30 days of enrolling in school. The previous year, that number (which has consistently been the highest among all North Carolina counties, according to the state Department of Health and Human Services) had sat at 4.9 percent, already up dramatically from just 1.6 percent in 2002-03. In the 2017-18 school year, the statewide rate was 1.2 percent; among the top 10 urban counties, New Hanover (2.3 percent) was the next-highest after Buncombe.
Although it’s relatively rare, chickenpox — which is highly contagious — can result in serious complications, including bacterial infections, pneumonia, encephalitis and even death, according to the CDC.
The issue, however, isn’t limited to North Carolina or even the U.S. Since 2009, the number of religious or philosophical exemptions has increased in 12 of the 18 states that allow them, according to a 2018 study published in the journal PLOS Medicine. And in Europe, where immunization rates among some groups have also dropped, outbreaks of measles, another highly contagious disease, caused at least 37 deaths in the first half of last year, the World Health Organization reports. The agency recently included “vaccine hesitancy” in a list of “Ten Threats to Global Health in 2019.”
In the U.S., hostility toward vaccines and fears of government intrusion date back at least to the 19th century, when states began passing mandatory smallpox vaccination laws. And in recent years, British gastroenterologist Andrew Wakefield and American pediatrician Bob Sears have triggered major controversies with their writings questioning the safety of vaccines. Wakefield subsequently had his license revoked, and last June, Sears was placed on probation by the California Medical Board, yet both men still have passionate, loyal adherents, and the underlying issues persist.
Legal exemptions
North Carolina allows two types of immunization exemptions. Medical exemptions, which must be documented by a physician licensed in the state, are rare. Instead, most of the Buncombe requests were based on religious beliefs. Within the passionate and opposing positions taken in the vaccination debate, however, the religious exemption has sparked its share of distrust and defensiveness.
Elio of MAHEC has about 28,800 Buncombe County students on her watch. North Carolina law mandates that all public, private and religious schools file an immunization report with the state Department of Health and Human Services within 60 days of the start of the school year, including the number of kindergartners, seventh-grade students and those new to North Carolina who have a valid medical or religious exemption from any required immunization. But schools aren’t required to specify which vaccinations students are being exempted from — and both the local Health Department and MAHEC say that’s also a concern.
Meanwhile, Elio is skeptical about religious exemptions in general. “All a parent or guardian needs to do is write a letter with the name of the child, their date of birth, and state that they have a bona fide religious belief. Nothing is required to back it up,” she explains. “That is considered compliant, and the child can attend school without immunizations.”
Mullendore, too, has doubts about the policy. “My sense, based on our experience in talking to people who take this exemption, is it is more of a personal philosophical belief or a mistrust of vaccinations than it is religion, but North Carolina law does not accept personal beliefs as a reason not to immunize,” she explains.
At least one Waldorf School parent takes issue with those objections, however. “The county very clearly thinks people are faking their [religious] exemption, that they are not religious people,” says this father, whose two kindergarten-aged children were granted religious exemptions. “We disagree with that. There are a lot of different ways to be spiritual and practice different faiths. Part of our faith and spirituality includes not putting toxic foreign substances into our bodies and our children’s bodies.” Because of threatening comments directed toward the school and parents following the chickenpox outbreak, he agreed to speak only on condition of anonymity.
Shared concerns
Mullendore wasn’t looking into a crystal ball when she told the county commissioners about the latest uptick in religious exemptions, but she says the chickenpox outbreak came as no surprise to her and other health professionals who’ve been watching those numbers with increasing concern. “We knew the stats were not good and that it was only a matter of time before an outbreak happened: We just didn’t know what it would be.”
In the 2017-18 school year, 10 schools in the county — all but one of them either private or charter — reported religious exemption rates of 10 percent or more. The Waldorf School had the highest rate: 19 of 28 kindergartners (67.9 percent). Across all grades, 110 of 152 students at the school (72.4 percent) had exemptions as of November. The lone noncharter public school on the list was Asheville Primary, at 24 percent.
“People tend to be with people with similar beliefs and lifestyles,” Mullendore observes.
Elio agrees. “Asheville is a place that embraces a healthy lifestyle: no bad chemicals in our foods or our gardens; we embrace what is natural, which is a good thing. But people who include vaccinating as unnatural is a challenge.”
The anonymous Waldorf parent, however, says, “The vaccination exemption rates were not a factor at all in our decision. We didn’t ask or know.” Instead, he explains, “We were attracted to the school because we felt that the teachers were incredibly in touch with creating an emotionally, spiritually safe and healthy environment for kids.”
He and his wife, both highly educated professionals, researched vaccinations while she was pregnant and based their decision on five factors: the ingredients in vaccines; their belief in building natural immunity to disease; experience with someone close to them who suffered a significant reaction they believe was caused by the polio vaccine; distrust of the pharmaceutical industry; and cases where a child contracted a disease despite getting immunized. His wife, he says, wasn’t vaccinated as a child but is very healthy.
“We asked around for pediatric practices comfortable with families that choose not to vaccinate,” he reveals. “We ended up with a pediatrician who told us to vaccinate but respected our decision not to. We feel strongly in our reasons, but we respect and understand that other people have other reasons, and that many people have reasons to vaccinate. We respect people’s medical decisions about their kids.”
Common goal
In her position as vice president of children’s services and chief of pediatrics at Mission Children’s Hospital/Mission Health, Dr. Susan Mims says she welcomes conversations with parents who have chosen not to immunize.
“I focus on our common goal: to keep their children healthy and safe. Every parent wants what’s best for their child, and they’re gathering information from all different sources. The first thing I try to do is understand what their concerns are, get their questions on the table, talk through their concerns and hopefully resolve them. I want them to feel heard. It is important to be in a trusting relationship with your pediatrician or family doctor and have respectful dialogue.”
Among the concerns Mims says she typically hears are pain from multiple shots, side effects of vaccines, ingredients in vaccines, the number of shots in the immunization schedule and whether all of them are really necessary. But the uncertainty and doubts, she and others maintain, are actually the ironic byproduct of the success of vaccines, which have sometimes resulted in several generations of parents having no knowledge or experience of the disease in question.
Mims says that in researching vaccine history, she sought out people raised before the development of vaccines that are now common. “In the 1940s, there was a polio outbreak in Hickory,” she notes. “Parents lived in such fear that their children would contract this disease and be crippled, paralyzed or face life in an iron lung. My father was in Western North Carolina, and he wasn’t allowed out of his house the entire summer. We have enjoyed growing up without that fear because of what a vaccine offers.”
Fears in collision
Nonetheless, fear is evident on both sides of the debate: parents who fear the ingredients in vaccinations or their side effects, despite years of rigorous testing, ongoing monitoring and scientific evidence to the contrary; and the medical community, which fears outbreaks of serious illnesses caused by high religious exemption rates in geographic clusters.
An ongoing measles outbreak in Washington state has produced 37 confirmed cases to date, almost all of them known to be unimmunized; on Jan. 25, Gov. Jay Inslee declared a statewide public health emergency. Washington and bordering Oregon both allow vaccine exemptions for personal and philosophical reasons. And in New York state, more than 200 cases of measles have been confirmed in observant Jewish communities since last October.
Measles is highly contagious: According to the CDC, 90 percent of unvaccinated people who come in contact with someone who has the disease will contract it. In the decade before 1963, when a vaccine became available, an estimated 400-500 people died of measles each year, 48,000 were hospitalized and 1,000 developed encephalitis.
Those numbers have declined precipitously since the vaccine was introduced. “I’m a doctor, and I have never seen a case of measles,” says Mullendore. “But we see what has happened in other communities with high rates of vaccine exemptions, and we know it can happen.”
Mims shares her concerns. “With so many exemptions, you’re rolling the dice,” she points out. “If someone with a disease or exposed to it comes into a community with low vaccination rates, they can spread the disease before they even know they have it. It’s the match that lights the fire.
“My personal passion escalated a few years ago when I saw a 4-week-old baby die of pertussis — whooping cough, a vaccine-preventable disease,” notes Mims. “At 4 weeks, this baby wasn’t able to be vaccinated, but having a vaccinated community around that baby would have been a very important means to prevent that death. Seeing a baby suffocate broke my heart. You hope it doesn’t take deaths or diseases to realize what vaccines do for us, but we are seeing pockets of outbreaks as we see more people choose not to vaccinate, and that’s what concerns me.”
According to the CDC, the varicella vaccine prevents more than 3.5 million cases of chickenpox, 9,000 hospitalizations and 100 deaths each year.
Quarantine order challenged
These medical professionals don’t believe that scaring parents or attacking their strongly held beliefs is an effective strategy. Yet attacked and frightened is precisely how the parents of unimmunized Waldorf School students say they felt when they received letters from Buncombe County Public Health Director Jannine Shepard imposing a 21-day quarantine that not only kept those children out of school but confined them to their homes.
“We were pretty shocked,” says the Waldorf father of two. “Our first reaction was scrambling to find in-home child care so we could work, and our next reaction was fear because of the way we were being described in the media, in online comments on those stories and in calls coming into the school. We were fearful for our children’s safety.”
These parents also felt that the county had overstepped its authority. Asheville attorney Lakota Denton represented 55 of the quarantined children and immediately started legal action on their behalf. Two weeks later, Superior Court Judge Richard S. Gottlieb ruled that the county could keep the children out of school but not confined to their homes.
“We thought the judge got it right,” says Denton. “But we are concerned it took a judge to tell our county Health Department they cannot confine over 100 healthy children to their homes for three weeks.”
Repeated attempts by Xpress to speak with other anti-immunization parents, and with local naturopathic and pediatric practices, were unsuccessful.
Finding common ground
Meanwhile, the underlying clash between individual and collective rights remains unresolved. And if every parent wants what’s best for their child, how do both ends of the spectrum come together to establish what is also best for the community at large?
“Before we had a child, my wife and I generally didn’t trust vaccines,” the anonymous Waldorf parent explains. “But then you see your little baby and the last thing in the world you want is for your kid to get sick, so you really have to weigh it out. For us, it came down to not wanting to purposely put toxins — whether for polio, whooping cough or chickenpox — in our kids’ bodies. I know people will say that not vaccinating your kids endangers everyone else. We feel that the risk of long-term health consequences from vaccines outweighs any other risk from not vaccinating.”
Mims, however, stresses that “Many, many studies have been done to prove the safety of vaccines. Nothing is 100 percent safe. But some of the information out there, especially with the internet, is not evidence-based. So all I can do is get that to my patients.” More than half of the families expressing concern about vaccines, she says, “do end up getting their children vaccinated” after receiving evidence-based information.
To that end, the Health Department teamed up last March with MAHEC and Mims to form the Immunization Coalition, inviting public health officials, doctors, nurses, school officials and parents to quarterly public meetings where they could sit down together and have dialogue. But while health sector participation has been high, outreach to parents, private schools and the faith community has been less successful.
Mullendore says that’s been frustrating for her. “I’m a doctor, a public health provider and a mother,” she notes. “I don’t want this to be an adversarial relationship. I want to have discussions with people who have made the decision not to vaccinate, to hear why and what brought them to that decision. I want to understand better so we can address and ease their concerns.”
Mims concurs. “There will be some folks we will never convince and whose minds we will never change,” she concedes. “But by making sure I get the large body of evidence that exists about the benefits of vaccines, and having a respectful conversation in a relationship where there is trust, many parents who were hesitant will choose to vaccinate their children. That’s the best we can do right now.”
Editor’s note: The online version of this article was updated at 11:52 a.m. on Feb. 11 to reflect that the baby who died of pertussis was four weeks old.
To learn more about the Immunization Coalition, contact Ellis.Vaughan@buncombecounty.org and ask to be put on the email list for notifications and updates.


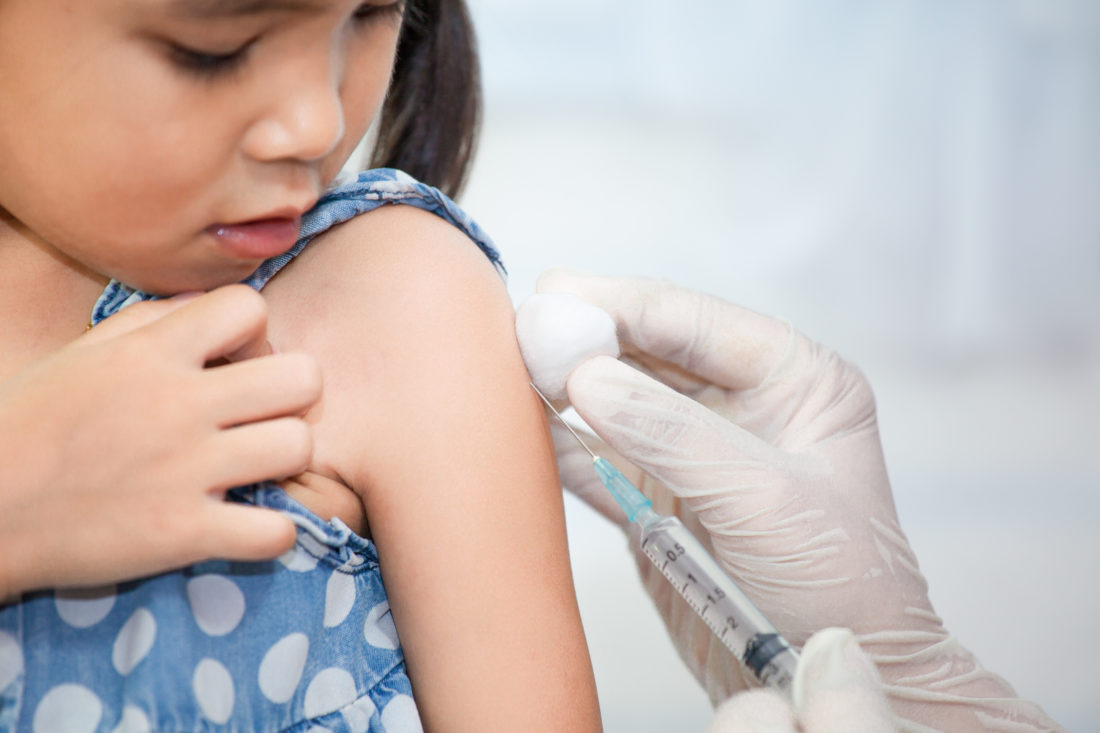
“We were fearful for our children’s safety.”
And to think, some people say irony is dead.
It is important to know that no safety testing is performed on vaccines and all of you doctors who think so should do some research rather than simply repeating what a pharmacy representative told you! The evidence is right in front of your faces. True history shows the corruption, fear mongering, and deception that was going on during the time of disease outbreaks. DDT should probably get some of the blame for the crippling of people since it was widely used. Graphs on infectious diseases show declines in diseases prior to the introduction of a particular vaccine. Give us good science or stop trying to convince the world the toxic ingredients in vaccines are safe.
It is important to know that this is a pack of lies.
https://www.historyofvaccines.org/content/graph-us-measles-cases
Hi again, Mr. Blissett. I’m guessing that the Pack of Lies you talk about refers to the true Scientific results you will never be able to find. Much truth can be found in the Cochrane files- try looking at THEIR pack of lies. It’s going to be hard for you to convince the world of the unvaccinated to vaccinate unless you have PMID numbers that back it up. You won’t. Accept the reality of the situation and make the decision to do no harm.
The Bring Back Diphtheria cultists can’t be convinced by facts. Maybe they’ll take notice when their little sunbeams die of preventable diseases, but it’s more likely that they’ll kill other people and not care.
“We feel that the risk of long-term health consequences from vaccines outweighs any other risk from not vaccinating.”
or: “We feel that polio and diphtheria are, y’know, old people diseases. We’re not into them these days.”
These parents are a) idiots; b) selfish idiots; c) idiots who endanger those with compromised immune systems. If your child develops cancer, are you going to revise your position on “toxic foreign substances” for chemotherapy? It’s almost as if diseases that regularly killed children in living memory mutated into a brain virus that convinces some parents that little Moonbeam and Solstice shouldn’t be vaccinated. So keep “religious” exemptions as long as one household at every school is chosen at random, infected with chickenpox, and confined to home quarantine with no medical assistance until it passes.
^^^THIS^^^
But maybe there is hope. Some kids of anti-vaxxer parents are coming to their own conclusions:
https://www.washingtonpost.com/health/2019/02/10/unvaccinated-teens-are-fact-checking-their-parents-trying-get-shots-their-own/?noredirect=on&utm_term=.3f14596655f1
Show us the randomized placebo controlled studies that prove the product is safe. There are none. You know it. How you feel is not relevant. Give us a good reason to inject ourselves with a list of toxins. (You know about them)
Show us the “declines in diseases prior to the introduction of a particular vaccine.” Given that the location of the Oteen VA used to be full of TB sufferers and now isn’t, the burden of proof is on the anti-vaxxers. How you feel is not relevant.
Which is more harmful to the population?
a) The measles vaccine
b) Measles
Which is more harmful to the population?
a) The pertussis vaccine
b) Pertussis
etc.
I expect an answer. The “vaccines are toxins, but deadly infectious diseases are natural” mindset is literally killing people.
Wake up. Do some real research. You have an answer: (1) Measles is a benign childhood disease that, when contracted, gives lifetime immunity. (2) Stanley Plotkin said himself that the pertussis vaccine caused an outbreak of whooping cough. Plotkin is the Godfather of Frankenstein science.
There is no need for me to continue discussing scientific approaches with people whose brains have been washed by big pharma. I am getting off your time warp.
Big pharma can make a whole lot more money selling iron lungs then it can by selling polio vaccines.
As for measles being a “benign” disease, tell that to the people who die from it — 110,000 people in 2017, most of who were children under the age of five.
The number of deaths from measles did drop by 80% between 2000 and 2017. Why is that? The measles vaccine. That you consider measles to be a “benign disease” speaks volumes and renders your “science” assertions meaningless.
It is so sad. Parents in third world countries often break down in tears when they learn that their children can get vaccinated against diseases that have killed others. Meanwhile among the Flat Earth Society in the US thinks it has the luxury of denying basic protection to kids
Yep, you’re in the “diseases are pure and natural” brigade, which makes you a disease carrier through non-biological means.
Agreed…and the advocates are so full of fear, brainwashing and sheep behavior…the list goes on and on. No wonder the US has such a “great” heath system…but hey, that’s how sheeples operate. Disturbing.
There is no need for you to make further assertions until you provide the evidence-Randomized Placebo Controlled Studies. I will not respond to any more silliness unless you first show the PMID numbers.
I’m quite disappointed with this very one sided article, that does not present verified information on what is known and legitimately published about the dangers of vaccines . . . Ms. West, I think you could’ve done better. You didn’t even mention the VAERS or the VICP which were installed in Mr. Reagan’s day in 1986 in the NCVIA (see link below). This legislation absolved Vaccine companies from ALL LIABILITY! (Big Pharma was in fact getting sued over vaccine injuries and threatened to stop making them) Yes, if you get a bad vaccine batch (or a good batch) and receive a brain injury–you cannot sue the Pharma company. You must sue the government thru VAERS and VICP. Although this is a long and difficult litigation, billions have been paid out. It is funded by extra charges on every vaccine sold.
Mr. Taylor speaks truth . . those ‘studies’ cited by doctors jabbing do not exist, or have been fully debunked by independent researchers investigating the ‘statistically enhanced’ data. . . . fyi, the alleged ‘studies’ are generally paid for BY the Pharma company–no conflict of interest there right? More disturbing is the very recent efforts by internet media to censor this important info.
Below are posted a few introductory links to supplement this MountainX article. . There is much more to be wary of with the vaccine protocols; Forced vaccination is called by many medical tyranny- ALSO, fyi Dr. Andrew Wakefield was character assassinated and de-licensed, but his research has never been disproven. . . ’twas a total reaction by the $35billion-with-a-B vaccine industry and others who enjoy the revenue. Also of interest is the report by CDC whistleblower William Thompson, which should have particular interest in this era of elevated racial sensitivity.
Those who chose to vaccinate should have freedom to do so by all means. All sides of this controversy need to be studied by parents, and updated info provided to Docs.
When a child gets measles, chicken pox and other childhood illnesses, they get actual immunity which mother’s can pass on to their offspring. Vaccines offer no such inheritable resistance. . . and some researchers are concerned the native immunity will be deteriorated for future generations.
Tell your docs and pediatricians to study more, they can start here:
https://en.wikipedia.org/wiki/National_Childhood_Vaccine_Injury_Act
https://en.wikipedia.org/wiki/National_Vaccine_Injury_Compensation_Program
https://en.wikipedia.org/wiki/Vaccine_Adverse_Event_Reporting_System
http://vaxxedthemovie.com/resources-information-group-organizations/ not-too-complicated intro to vaccine injury and politics
VAXXTER.com Dr. Sherry Tenpenny, also character assassinated but never disproven
https://childrenshealthdefense.org/
. . . AND< read the side-effects small print on the vaccine box . . . . .
Some MountainX vaccine history:
https://mountainx.com/living/032608vaccinate/