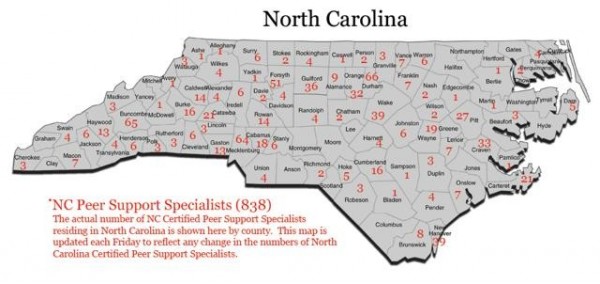
Help is here:As of March 21, there were 838 peer support specialists in North Carolina, 65 of them in Buncombe County. Map courtesy of the Peer Support Specialist Program at UNC-Chapel Hill
Kevin Mahoney knows the journey. During his 20 years in the Air Force, he reveals, “I drank a lot: I’ll be perfectly honest.” And after he returned home, “I started waking up at 3 a.m. feeling hopeless, night sweats, nightmares. All these mental health symptoms started ganging up on me, and I tried to self-medicate. I had PTSD and didn’t even know it.”
It was only later, he continues, “when I’m getting therapy and alcohol-withdrawal medication, that I could come to a better place.”
But Mahoney also knows the system. Whether it’s finding a counselor or working with mental health agencies, he knows where to go and what to do. A peer support specialist since 2010, he now helps others navigate that system. Besides completing the required 40 hours of training and receiving credentials from the state and the Behavioral Health Resource Program, however, peer support specialists have one other advantage: They’re in recovery from mental illness and/or substance abuse themselves.
“It’s like the old belief of ‘Talk the talk and walk the walk,’” Mahoney explains. “People really begin to trust you, knowing that you may have come from a very similar place.”
The concept of peers helping peers is nothing new in health care. Consumer satisfaction teams were first developed in Pennsylvania in the 1960s, so people interacting with the health care system could share their experiences with one another. In North Carolina, the idea of peer support specialists didn’t get much attention until 1987, and it was another 20 years before the state established a training curriculum.
Since then, the field’s growth has been impressive. By 2009, there were about 250 certified peer support specialists in the state; in the last four years, that number has more than tripled. As of March 21, there were 838 certified peer support specialists in North Carolina, 65 of them in Buncombe County.
Mahoney is part of an “assertive community treatment team” at RHA Behavioral Health Services, a group practice specializing in psychiatry, social work, nursing, substance abuse and vocational rehabilitation. To encourage independence, the team teaches coping skills while engaging clients in normal daily routines and healthy social interactions. But the peer support specialist can offer something his colleagues probably can’t.
“We can provide therapists and case managers and medical staff to help the person, but at the end of the day, none of those people are going to really truly know what it’s like to be in that particular situation, whereas a peer support specialist usually does,” says Sandy Fuete, RHA’s director. “The peer support specialist may be the only one on that team that can say, ‘Hey, I get that. I know how you’re feeling in that situation. That’s exactly where I was.’”
Social worker Andrea Morris, who’s trained more than 250 peer support specialists locally, says interest in the profession is growing. Almost 20 people signed up for a recent training she led at October Road Inc., an Asheville-based mental-health and substance-abuse care provider.
“There’s been a lot of demystifying about what a peer support specialist actually does. Providers have a better understanding of peer support,” Morris explains. “The community is accepting and embracing the integrity and value of someone that has traveled the path to wellness understanding the service they might provide to someone who is currently experiencing that.” For her, the emergence of the field is a testament to “the resilience of the human spirit.”
Official recognition by the state and Medicaid (which now reimburses agencies providing this service) is a key step, says Fuete. “They’ve made a nod to acknowledge that peer support is valuable. I think it has brought North Carolina into thinking more about the concept of recovery in terms of both mental health and substance abuse needs.”
But Fuete, Morris and Mahoney all maintain that what’s needed is a deeper shift in society’s attitude toward recovery.
“When a person is in the midst of significant mental illness or substance abuse symptoms, hope is often the one thing they’re lacking,” notes Fuete. “There’s so much stigma around mental illness and substance abuse that, often, people in the community could just not even conceptualize that people with a mental illness diagnosis could work and help other people. There’s a lot of stereotypes.”
Mahoney agrees. A person, he stresses, is “not a set of symptoms.” For him, however, the most important part of his job is giving the people he works with a glimpse of what they might become.
“My pathway may not be the same as someone else’s, and everybody has their own journey, but it shows them that it’s possible to find a way.”
— Send your health-and-wellness news and tips to Caitlin Byrd at cbyrd@mountainx.com or mxhealth@mountainx.com, or call 251-1333, ext. 140.


Before you comment
The comments section is here to provide a platform for civil dialogue on the issues we face together as a local community. Xpress is committed to offering this platform for all voices, but when the tone of the discussion gets nasty or strays off topic, we believe many people choose not to participate. Xpress editors are determined to moderate comments to ensure a constructive interchange is maintained. All comments judged not to be in keeping with the spirit of civil discourse will be removed and repeat violators will be banned. See here for our terms of service. Thank you for being part of this effort to promote respectful discussion.