A new pilot program that started this summer helps people with opioid use disorder to initiate medication-assisted treatment in Mission’s emergency room, and then coordinates follow-up care.


A new pilot program that started this summer helps people with opioid use disorder to initiate medication-assisted treatment in Mission’s emergency room, and then coordinates follow-up care.
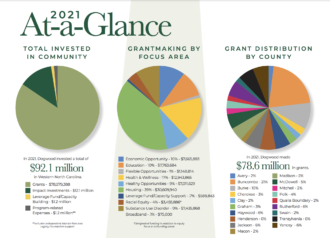
In total, Dogwood approved 287 funding requests of the 354 grant applications in 2021. The nonprofit also reports that it added 21 new staff members to the organization.

“This is a workforce who has that trust, connection and inherent knowledge of what people are experiencing and are trained and equipped to address individual and community health,” says Evan Richardson, MAHEC’s director of community health integration. “This is a workforce that can really make an impact.”

Tens of thousands of people across the experience lingering illness after a bout with COVID-19. The condition, called post-acute COVID-19, may impact up to 60% of people previously infected with the coronavirus.

The Buncombe County Board of Commissioners recognized April as Child Abuse Prevention Month, and Dogwood Health Trust opened on online grant application portal. Read about these items and more in this week’s wellness roundup.

Early data suggests monoclonal antibody therapies may reduce hospitalizations in people at high risk for severe COVID-19 complications by 70%. Limited supplies are now available in Western North Carolina.

Even with health insurance and ample provider availability, fat discrimination by providers can be a barrier to care for overweight people.

“Human beings just aren’t designed to be isolated in perpetuity,” says Rhonda Cox, executive vice president and chief population health officer at Vaya Health. But that’s exactly what many have had to endure over the past 10 months, and the strain is showing up in the region’s mental health system.

“We’ve got an epidemic within a pandemic,” says Kevin Mahoney with the Mountain Area Health Education Center. Social distancing, job losses and drug contamination associated with COVID-19 have all complicated local efforts to manage the impacts of opioid use.
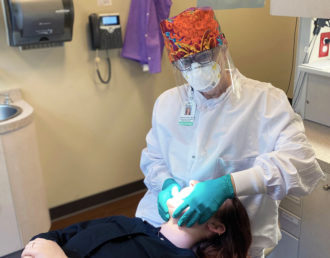
While regular dental hygiene may be able to wait a bit longer, some dental appointments can’t be put off. What steps are local practices taking to ensure the health of staff and patients during the coronavirus pandemic?

The pandemic has isolated rural residents with mental health needs. But these North Carolina providers are finding creative ways to connect.

As confirmed by Mission spokesperson Nancy Lindell on June 11, the health system’s legal representatives have chosen not to file an objection regarding how a pre-election hearing was conducted. The National Labor Relations Board will now consider testimony to determine what nurses would be represented by the union, when the vote will take place and how employees will be allowed to cast ballots.

“You don’t have to be a psychiatrist to know that when you take away people’s routines and jobs, it’s difficult for them, especially if they have a mental illness,” says Brian Ingraham, CEO of Vaya Health. New federal funding will help two Western North Carolina agencies expand mental health services, some directly related to the pandemic and the rest addressing overall behavioral health issues.

Local medical experts weigh in on the effects of screen time on toddlers and children.

Dr. Jeff Heck, CEO of Mountain Area Health Education Center, shared his take on threats to health in this area, remarking, “Ironically, what makes Western North Carolina so desirable — the beauty of our predominantly rural region — also makes us vulnerable to a variety of challenges that are part of a national rural health crisis.”

From 2010 to 2018, “Our black infant mortality rate has increased from 11.7 to 15.1 deaths for every 1,000 babies born,” Hannah Legerton told Buncombe County commissioners on Dec. 3. That means that black babies in Buncombe County are four times as likely to die before their first birthday as white babies. And since infant mortality is a leading indicator of population health, health officials say, those numbers bode poorly for the wellbeing of African American county residents. Collaborative efforts are seeking to address the underlying issues driving inequities in health outcomes.

Over 100 members of the community attended Let’s Talk Opioids, described as a “community update and conversation on opioid crisis response in Buncombe County.” The standing room-only crowd listened as in-the-trenches experts presented information, including the Mountain Area Health Education Center, Vaya Health, Asheville Fire Department, Buncombe County Health and Human Services and the N.C. Department of Justice.

“Often we can reach folks better through technology than we can face to face,” says Shane Lunsford of the Center for Psychiatry and Mental Wellness. As telehealth service offerings and technological capabilities expand, providers around the region are excited about the possibilities of new models of seeing patients and providing care.

Local elected officials say they want Asheville and Buncombe County to be considered a breastfeeding-friendly community to boost lifelong health for residents, but does that intention line up with today’s reality for nursing moms?

A new statewide report on women’s health was unveiled June 25 in Asheville. Mercy Urgent Care is now an in-network service provider for eligible veterans using Veterans Administration benefits. The Asheville Yoga Festival will be held Thursday-Sunday, July 25-28, and one-day passes and a discount for Buncombe County residents are now available.

A new play for children, It’s Just a Pill, premiered at A-B Tech’s Ferguson Auditorium on March 8. The 55-minute musical confronts the opioid epidemic from the perspective of a 10-year-old girl. The production will now travel around North Carolina to reach over 4,000 young people.