There’s a widespread challenge affecting our neighbors and families — and not many people are talking about it.
Many people in Asheville and the rest of the country are struggling with the difficulties of caring for someone else. According to the Centers for Disease Control and Prevention, about one in four adults has provided some type of family caregiving within the last month, and the problems and stresses that come with that are many.
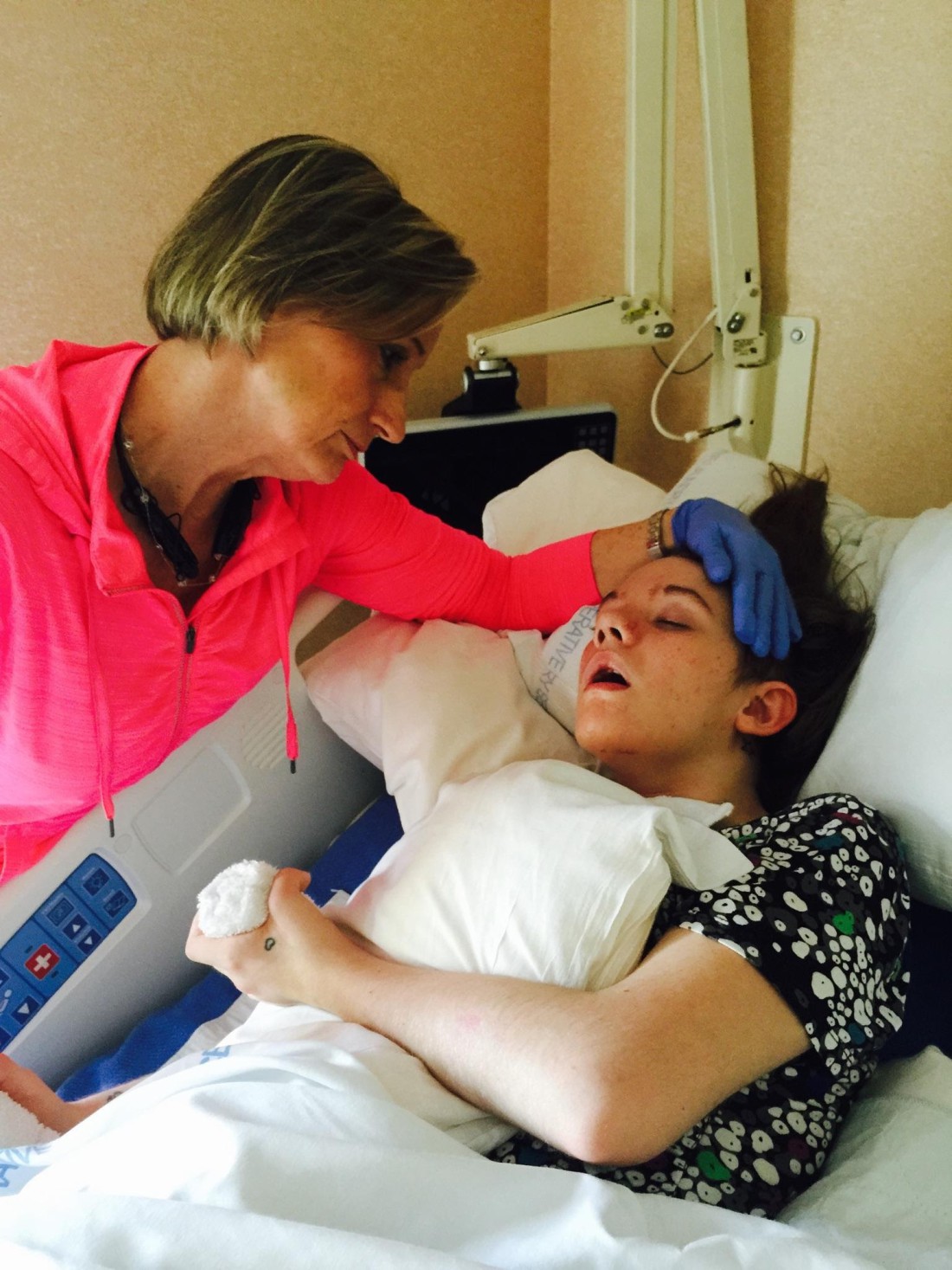
Take the case of Robin Embler of Asheville. Almost three years ago, her daughter suffered a traumatic brain injury, which thrust Embler into a caretaker role.

“My daughter Victoria was 22 years old and four months when she was a pedestrian hit by a vehicle traveling more than 45 miles an hour,” explains Embler. “Beautiful girl, honor student and mother of now my six-year-old grandson.”
Embler now finds herself engaging in almost 24-hour care — changing clothing, preparing smoothies, administering medications, brushing teeth, advocating, coordinating, engaging in therapeutic activities and an endless number of other daily tasks that require more time than she has.
It takes its toll. As a caretaker, Embler says she has lost relationships, financial stability, time for herself and everything that goes along with that. But she knows she’s not alone.
“This is not just a local story,” she says. “It’s a state story, it’s a national story.”
Nation of Caretakers
Carol McLimans, a family caregiver specialist at the Area Agency on Aging at Land of Sky Regional Council, has been working with family caregivers for over 15 years.

“One person ends up being the primary caregiver even in a large family, for the most part.
She explains that often people like Embler are suddenly thrust into a caregiving role when a loved one becomes seriously injured due to an accident or illness. And it may be a role that becomes a life-long commitment.
“I see so many people caring for someone with dementia, and they’re going to be doing that for five to 20 years,” says McLimans. “It’s a long, long haul. I also know that the caregivers of special needs children also suffer from a lot of stress. They have a whole lifetime of caring for them.”
While anyone can suddenly find themselves in a caretaker role, most caregivers tend to be “in their late 40s, maybe early 50s, caring for ill parents or children, and they’re employed,” says McLimans.
Caretakers usually have to manage the stress of their full-time job, only to go home to a second job. “All the reports say they’re working about 20 hours a week caregiving,” she adds.
Stressful Work
Caretakers are susceptible to intense emotional and physical stressors. Martha Teater, a marriage and family therapist in private practice in Waynesville, hears about the fatigue firsthand.
“Watching someone you love go through a period of decline or health challenges or deterioration of some sense — whether it’s dementia or whether you’re caring for a child who has challenges, or a partner or someone, no matter what the relationship is — it’s emotionally taxing and often physically taxing,” she says.

The impact of caregiving can be grave for the ones that give.
McLimans shares the sobering news that “caregiving is a public health hazard because we know that caregivers die before the person that they’re caring for, fairly often.”
Shantel Sullivan, assistant professor in the department of social work at Western Carolina University, notes one Stanford study that found “around 40 percent of certain caregivers end up becoming ill and passing away before the person they are caring for.”
One way a caretaker suffers is by the constant need to sacrifice.
“There are a lot of studies that show that the individual, the caregiver, neglects their own health,” says McLimans. “They don’t go to the doctor, they don’t go to their own appointments. They missed their own appointments because they’re so busy caring for the person that they’re caring for, or they’ll put their own surgery on hold because they have no one to care for [their loved one].“
Jack, a family caretaker who asked that we not use his real name, attests to the stresses of caretaking and the ways that it became a significant health risk for himself. He moved to Asheville over a year ago when his mother’s health deteriorated.
She “needed somebody to be here: cook the meals, do some cleaning, and just make sure that everything was day-to-day okay,” he recalls. “Things seemed to go pretty well.” But months later, Jack’s mother needed even more assistance when she developed a sudden infection.
“It involved me really doing a lot of care,” he says. “Getting up in the middle of the night, every night. Then having to clean up after, give her a bath, clean up the bathroom; just really, I was out of my league. I think the problem for me was that the day started around nine o’clock [a.m.] and it ended around 10 o’clock [p.m.], seven days a week.”

According to the National Institutes of Health, “Caregiving has all the features of a chronic stress experience.”
Sullivan says, “It is not just a one-point incident. This is something that’s occurring on a daily basis. It’s sort of that ongoing wear and tear of the relationship and the emotional demands and physical demands and social demands of a caretaker.”
Teater agrees, adding, “People often have sleep disruptions and difficulty being able to show up at work and be as productive as they want to be. There may be financial challenges. There may be social isolation. There could be anxiety and fear with it. They may feel like they aren’t really trained and equipped in how to do this. They are probably not professional caregivers, but they are being called into doing things that are really difficult on an ongoing basis … . So they’re juggling a part-time job along with a full-time job.”
In Jack’s case, he already had a pre-existing heart disorder that caused his heart to occasionally beat fast for a couple of minutes. “Well, from all the stress it just kept getting worse and worse — last winter it was getting about 200 beats a minute, and it would not go away,” he says. “I remember my last episode lasted about an hour before I decided to call 911. Well, we kept it under control with medication, and I was back at it. So that was the lesson I learned: It does affect you. The stress level creeps up on you, and it’s real. I heard many times that it’s stressful, and I thought, ‘Well, we’ll see. I’m not too worried.’ But it is.”
Denise Young, regional manager of the Alzheimer’s Association Western Carolina Chapter, has been witness to many caretakers’ struggles.
“We find the caregivers are getting sick a lot more often,” Young says. “They are having trouble sleeping. Oftentimes, they are gaining weight and really just expressing that they are feeling such hopelessness. You just see signs of depression. They become really irritable and just feel really hopeless in their role as a caregiver.”

Financial Stressors
Even though Jack’s caretaking duties led him to need medical care, he reflected that “we’re very fortunate that things have worked out that money was not a huge problem. I can’t imagine it for people that don’t have the funds. That would be horrible. It would really add to the stress.”
Sadly, most caretakers suffer some financial stress brought on by caretaking.
A 2016 study conducted by the AARP indicated that family caregivers almost always take a huge financial hit on their income and out-of-pocket expenses.
“The money is very slim, the help is very slim,” explains Embler. “In my situation, my daughter was four months too old to qualify for help, so she’s fallen through the cracks. Insurance doesn’t even scratch the surface of what she needs. And that’s what families are forced to do. Become a caregiver — bringing their loved one home, without support.”
Young says, “We do hear a lot of that feedback from caregivers that they are very frustrated with the fact that Medicaid doesn’t cover certain expenses that they have and the fact that we are so limited on facilities — assisted living facilities or long-term care facilities that actually accept Medicaid.”
“And I think that is going to be an ongoing battle for us, and our public policy is doing everything we can to address that.”
Respite and Relaxation
Experts say that one of the best ways for caretakers to recharge is to find help and schedule time for themselves.
McLimans notes that caretakers “need to plan something … not something that they should or have to do, but something that they truly want to do. They should plan to do that weekly or monthly. What they tend to do if they get any funds is wait until a real crisis happens. They’ll wait until things get worse.
“Typically, they think a couple things,” she says. “‘No one else can do it right’… .They’re convinced that they don’t need the help … . Or it’s like asking for help is a sign of weakness.”
Caretakers need more than just taking an occasional break. Young says support at every level is necessary to avoid caretaker exhaustion.
At the Alzheimer’s Association, she says, “We try to help them just to set some reasonable goals around that and accept that they are going to need help from other people and give them the resources that they need to help build a care team around them. Some part of that is just helping to connect them with people they trust, whether it is a friend or a coworker. Sometimes it is even a neighbor or someone from their church that they can connect with and have someone to talk to about what they are going through.”
But receiving help doesn’t mean the caretaker is completely unburdened.
Anne, a resident of Asheville who prefers not to use her real name, looks after her son, who sustained a traumatic brain injury almost 15 years ago and was subsequently diagnosed with bipolar disorder. She says the support team she has put together is the key to her avoiding burnout, but there are other levels of stress to deal with.
“Unlike a lot of people, we do have a lot of support from the mental health system and through Medicaid. So he has a lot of direct staff and personnel that shoulder a lot of the responsibility,” she explains.
But, she adds, “When you get enmeshed in the system of health care and direct services and all that stuff, while I have been very blessed by it, it’s exhausting to try. You know, they want you to come and speak to this company and that company and that agency and this agency in government. It’s just a whole other level of stress. And the advocacy was full time. It was full time.”
“That’s another thing,” says McLimans. “If someone is placed in a facility, [caretakers] still need to be advocates. You still get burned out. You’re still going every day and checking up on them. They don’t get to give up their caregiving.”
Caretaking Tips
To reduce the risk of burnout, Teater advises caretakers to “place a higher priority on getting good sleep and having good relationships and getting some respite and finding pockets of support wherever they can.”
Other suggestions from all those interviewed include practicing gratitude, communicating with family, taking classes and finding the right support group. Even a service animal can be a powerful member of the support team. Victoria’s service dog in-training has already made a difference, says Embler. “Louie weighs five pounds, but he makes 5,000 pounds of difference.”
One example of an educational community program utilized by caretakers can be found at the Osher Lifelong Learning Institute at UNC Asheville.
OLLI Executive Director Katherine Frank says, “People use OLLI as a way for caregivers to get time for themselves, even if they bring the person they are caring for. In many instances, caregivers are spouses or partners of older adults. So a program like ours that provides classes and social opportunities can provide a way for someone who is maybe unexpectedly in a position of a caregiver the opportunity to be with other adults and keep their own mind stimulated and to be around other people who may be facing these kinds of issues.”
As for support groups, McLimans recommends a large list of agencies, programs, professionals, support groups and other caregiving resources in Buncombe, Henderson, Madison and Transylvania counties. The list is maintained by the Land of Sky Regional Council and can be accessed at landofsky.org.
Changed Forever
Even though caretakers have many struggles, they still can find the experience rewarding and life-changing.

Victoria is now “medically stable and totally aware of her surroundings … beginning to make sounds … and using a little sign language,” says Embler. “I’m so blessed that my daughter is still with me. I believe there were angels that day, picking her up off the pavement. I really, really do. God’s got a plan and a purpose in the midst of it all. We’ve got to make a difference, not just for Victoria, but for others like her who fall through the cracks.”
More Info
Alzheimer’s Association, Western Carolina Chapter
Caregiver Resource Directory
Confident Caregiver Series
828.251.6140
Osher Lifelong Learning Institute
Victoria Faith


Before you comment
The comments section is here to provide a platform for civil dialogue on the issues we face together as a local community. Xpress is committed to offering this platform for all voices, but when the tone of the discussion gets nasty or strays off topic, we believe many people choose not to participate. Xpress editors are determined to moderate comments to ensure a constructive interchange is maintained. All comments judged not to be in keeping with the spirit of civil discourse will be removed and repeat violators will be banned. See here for our terms of service. Thank you for being part of this effort to promote respectful discussion.