Multiple times a day, the Buncombe County Emergency Services Department is dispatched to 911 calls for drug overdoses.
Nearly all of the overdoses are from opioids — heroin, fentanyl or prescription drugs like OxyContin or Percocet. An average of nine people died from a drug overdose each day in 2020 in North Carolina, the N.C. Department of Health and Human Services announced in March. The BCEMS’ post-overdose response team, or PORT, has responded to 900 opioid overdoses in the county since January 2021, says lead paramedic Claire Hubbard.
As of last month, PORT had a new tool for helping an individual suffering from an opioid overdose: medication-assisted treatment, or MAT. The program is called Bridge to Care and is a collaboration between PORT and Mountain Area Health Education Center.
MAT is an evidence-based treatment for opioid use disorder, according to the Centers for Disease Control and Prevention. The treatment involves taking a medication — either buprenorphine, methadone or naltrexone — along with counseling to address the addiction.
Since March 7, PORT has referred 17 people to Bridge to Care following overdoses, says PORT’s peer support specialist Justin Hall. (PORT has at least 85 people on its caseload, meaning it connects clients to support services after an overdose.)
The pilot is meant to reach people who might otherwise not have resources to access MAT. “Who is most at risk of dying [of an overdose]?” Dr. Shuchin Shukla, family physician and opioid educator at MAHEC who helped develop the MAT pilot. “Let’s go and give them the lifesaving treatment — not say ‘Here’s a pamphlet with an appointment’ or ‘Here’s a phone number, call this.’”
Shukla continued, “These folks are uninsured. They don’t have phones. They’re living in tents. … We’ve got to skip all these barriers and bring [MAT] to them.”
Timing is everything
PORT began in November as a pilot program with BCEMS, and it connects people to further assistance within 72 hours of an overdose. Some individuals need stable housing or a connection to mental health servers. Others want to begin treatment for their substance use disorder.
However, an authorized health care provider is required to administer MAT, according to the N.C. Medical Board. Many people weren’t able to get a dosage immediately following an overdose, would start going through withdrawal symptoms and use again, explains Hall. And the cycle would continue.
Opioid withdrawal is “one of the worst feelings most people could feel,” says Shukla. “Runny nose, teary eyes, super-achy, and at worst, bone pain, feeling very uncomfortable — like skin crawling — can’t sleep, can’t eat and a lot of [gastrointestinal] stuff, meaning nausea, vomiting, diarrhea, cramps.”
Shukla continues, “It’s pretty awful because you can’t sleep but you’re super-tired. You can’t eat, but you’re getting dehydrated because you’re vomiting and having diarrhea. … And, man, if you use an opioid, all that gets better pretty immediately.”
This is a dangerous circumstance, says Hall. People would “end up overdosing again, because they were trying to deal with the withdrawals and actually died,” he says.
Most facilities that provide MAT are open Monday through Friday during regular business hours, explains Hubbard. Someone who has an overdose during off-hours may have to wait days to begin MAT and this could derail their recovery process, she says.
How it works
The Food and Drug Administration has approved several different medications for opioid use disorder. BCEMS currently administers Suboxone — a combination of naloxone (the medication that reverses overdoses, also known as Narcan) and buprenorphine, according to the National Alliance on Mental Illness.
“Buprenorphine works by stimulating the same receptors [as other opioids], but it does it in a different way than heroin, oxycodone, morphine [and] fentanyl,” Shukla says. Buprenorphine is a schedule III controlled substance regulated by the U.S. Drug Enforcement Administration; the FDA approved Suboxone in 2002.
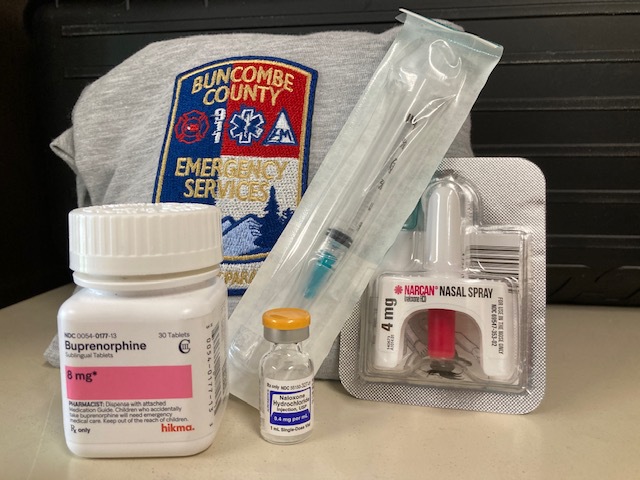
Medication-assisted treatment is an evidence-based treatment for opioid use disorder, according to the Centers for Disease Control and Prevention. Photo by Justin Hall
MAT is safe for use for “months, years or even a lifetime,” according to the U.S. Department of Human Services Substance Abuse and Mental Health Services Administration.
“That’s the beauty of buprenorphine and Suboxone — they fix that feeling [of withdrawals] without the risk of hurting the person,” says Shukla.
Connection to further treatment
PORT responds to all overdose 911 calls alongside the other first responders, who may be the ones who administer Narcan. First responders then leave the scene and go back into service responding to other calls.
The community paramedics stay. While “acknowledging the fact that they were given a medication that responds to opiates and they did overdose on opiates,” Hall explains, PORT broaches various resources for both harm reduction and recovery. “If they are interested in getting onto Suboxone, we can facilitate that,” he says after assessing the individual for withdrawal symptoms.
PORT has referred 17 individuals to Bridge to Care to begin MAT “either immediately after the overdose or sometimes we wait until the next day,” explains Hall. “Basically, we’re waiting to see where their withdrawal symptoms are.” If not administered at the right state of withdrawal, MAT can potentially make someone feel “even worse,” he says — which can lead to using opioids again to feel better.
After providing a first dose of Suboxone, the community paramedics make a plan with the individual to return the following day for redosage. “Our paramedics are prepared to go out every 24 hours and dose an individual for up to five days,” Hall explains. During this time, PORT helps schedule an appointment for the patient at MAHEC in the coming days.
In December, Dogwood Health Trust awarded MAHEC a $499,000 grant to provide buprenorphine at no cost in the Family Health Center, a primary care clinic. The grant will support up to 60 uninsured patients referred through the PORT program for up to one year, MAHEC spokesperson Jennifer Maurer says. And PORT can bring people to these appointments — a crucial component, since not having transportation can be another barrier to receiving treatment.
Two of the 17 patients who started MAT through PORT haven’t shown up for their MAHEC appointment to continue treatment. Hall says, “I don’t think they were fully ready to give up their drug of choice.” But the community paramedics will still keep in touch and continue to offer MAT as a treatment option. “When they’re ready to make that reconnection to MAHEC then we can do that as well,” he says.
The long-term plan is for the 15 people in Bridge to Care to take additional steps toward recovery via wraparound services with the assistance of other nonprofits in the county. Two individuals have entered detox, Hall says, and two have started jobs.
“We’re running the ship pretty tightly right now, where we’re making sure people don’t fall through the cracks,” adds Shukla. “These are the people who fall through the cracks the most.”



Before you comment
The comments section is here to provide a platform for civil dialogue on the issues we face together as a local community. Xpress is committed to offering this platform for all voices, but when the tone of the discussion gets nasty or strays off topic, we believe many people choose not to participate. Xpress editors are determined to moderate comments to ensure a constructive interchange is maintained. All comments judged not to be in keeping with the spirit of civil discourse will be removed and repeat violators will be banned. See here for our terms of service. Thank you for being part of this effort to promote respectful discussion.