Women’s relationship with their breasts is complicated. It includes apprehension about development, insecurity about size and shape, uncertainty about how to enhance/reveal/cover up/support them — and then, post-middle age, concern about how well they’re holding up.
But nothing compares to the alarm felt when detecting a suspicious lump while taking a shower, the anxiety while awaiting the results of a mammogram or the heart-stopping terror triggered by the words “It’s cancer.”
No one knows this more intimately than the medical professionals who interact with patients in the rapidly evolving field of breast health: geneticists, genetic counselors, radiologists, oncologists and nurse navigators.
“Most breast cancers require a combination of different treatments, and the order and combination of those things is a whole lot more complicated today than ever before,” says Dr. Blair Harkness, a gynecological oncologist at Hope Women’s Cancer Centers, an arm of Mission Health. “That is not a negative: We know so much more today about the different subtypes of breast cancer. Treatment is much more individualized, based on the biology of the different types of breast cancer.
“You have to identify exactly what you’re dealing with first, what kind of cancer, and then you can put together the plan and order of things. It’s an important multidisciplinary team: genetics, surgery, medical oncology, radiation oncology, radiology, pathology. We all work together.”

Dr. Jennifer McAlister, a breast surgeon at Pardee UNC Health Care, concurs. “Each patient at Pardee receives multidisciplinary care,” she explains. “The entire breast cancer team is on one floor in the cancer center, so it’s easy for us to talk about specific cases. We also have a multidisciplinary tumor board that meets weekly to discuss all cancer cases. That team includes a radiologist, pathologist, medical oncologists, radiation oncologist, surgeons and palliative care.”
Meanwhile, the current pandemic has further complicated efforts to diagnose and treat the disease (see sidebar, “Breast cancer in the time of COVID”).
Baselines and gray areas
Physicians encourage adult women of all ages to perform monthly breast self-exams. At age 40, women are advised to get a first baseline mammogram. “Mission recommends an annual screening beginning at 40, because that reduces your risk of dying from breast cancer by 40%,” says Dr. Sheri Fleeman, assistant medical director of breast imaging at Mission Health. “One out of 6 breast cancers are diagnosed in the 40-to-49-year-old age range. Our goal is to find cancers early, treat them early and save as many lives as possible, and we feel like we can do that best if we start at 40 and do an annual.”
There are exceptions, however. “We recommend a baseline mammogram at age 40 unless a patient had a direct family member previously diagnosed with breast cancer,” said Linda Richards, who has since retired as administrative director of cancer services at AdventHealth Hendersonville (formerly Park Ridge Health). “For example, if a woman’s mother was diagnosed with breast cancer at 42, the recommendation for baseline for this woman would be 32: 10 years prior to the family member’s diagnosis.”
Documenting family medical history is now standard procedure: For their first appointment at any practice, all new patients complete a lengthy questionnaire. When that information raises a red flag, patients may be referred to a genetic counselor.
“Providers are becoming a lot more proactive asking about family history, and if there is cause, they may suggest an appointment at a genetics center,” says Mission Health’s Carolyn Wilson. “We see people here for all types of indications, but the biggest area of growth, here and at all genetics centers, is in the area of inherited cancer,” notes Wilson, one of six genetic counselors at the region’s only such facility.
“We know that about 10% of cancer is genetic, so it’s very common for people who either have a family history of cancer or a new diagnosis of breast cancer or another type of cancer to be referred to genetics.” Determining if they might be in the genetic group, she continues, “can certainly impact their screening, their treatment and medication choices.”
Patients can expect the first appointment with a genetic counselor to run from 75-90 minutes. In addition to reviewing both personal and family cancer history, counselors will discuss the benefits and limitations of genetic testing. The process, says Wilson, “is kind of complicated, and the results are not always black or white. We sometimes find an uncertain genetic change, which is not the same as a positive. … You might not get a yes or no answer.”
For those who decide to go ahead with it, the process involves either a blood or a saliva test. It takes two to three weeks to get the results, “And if anything comes back positive or uncertain, we are happy to meet again to review the information,” says Wilson. “The report and a detailed letter are sent to them and their provider, so together they can map their next steps.”
3D imaging
Even for those who test negative, however, the center creates a risk assessment based on personal and family history. Nongenetic factors that increase breast cancer risk include increased breast density shown on mammograms, having one’s first period at a young age, having children later in life or not at all and hormone replacement therapy.
“If a person’s lifetime assessment risk for breast cancer is greater than 20% based on these computer-based models, they are recommended to follow high-risk breast screening, which includes an annual mammogram and breast MRI,” notes Wilson.
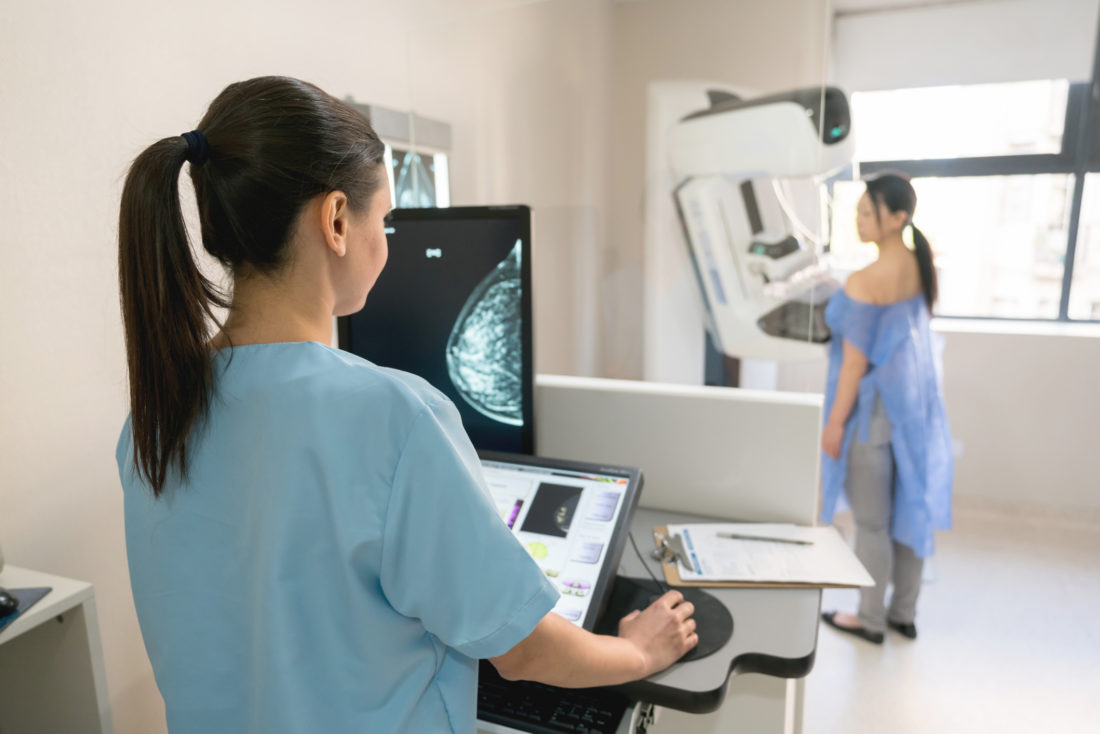
And while mammograms are still the procedure most laywomen think of when it comes to getting naked and having your breasts squeezed flat between plates, breast imaging is a more accurate description of the many tools radiologists currently use to “see” the breast.

“The 3D mammogram,” explains Dr. David Onofrey of AdventHealth’s Medical Group Breast Center, “creates a better image by pulling multiple X-ray images in just 10 seconds. A computer puts the images together, and this produces concisely focused three-dimensional images throughout the breast. Studies show that 3D mammography detects slightly more breast cancers than standard.” AdventHealth, Mission and Pardee all perform this procedure.
At Pardee, notes McAlister, all mammograms are now 3D. “In patients with dense breast tissue, we know that 3D mammograms find smaller masses or cancers that could be hidden on traditional 2D mammograms,” she says. “When the breast tissue is dense, it tends to overlap on itself and can be difficult to read.” The 3D imaging “allows us to view the breast in ‘slices,’ so there is less risk of missing something small.”
Another useful technology for women who have dense breast tissue — a condition that, when discovered in a standard mammogram, must be reported to both physician and patient — is the 3D whole breast ultrasound, or ABUS. The procedure, says Fleeman of Mission Health, uses sound waves to take 3D pictures of the breast. “This is helpful because the breast is composed of fatty tissue and glandular tissue. The more glandular tissue you have, the denser your breasts. On mammograms, the fatty tissue is black and the glandular tissue is white. Cancers also show up as white, so in dense breasts, it’s like looking for a polar bear in a snowstorm. ABUS is a totally different way of looking at breast tissue, and in patients with dense breasts it can pick up cancers a mammogram might miss.”
Yet another advanced tool is a breast MRI, which requires an IV to provide contrast. A more expensive test, it’s reserved for high-risk patients, says Fleeman.
Targeting tumors
If a tumor is detected, the next step would be a biopsy, and here too, advanced technology plays a role. “The 3D-guided biopsy provides the radiologist with a clearer, more detailed image, allowing precise, accurate sampling of the tissue,” explains Lisa Gundersen, clinical operations director of cancer services at AdventHealth. It’s also more comfortable for the patient, she continues. AdventHealth, Mission and Pardee all offer this procedure.
For patients diagnosed with cancer, the interdisciplinary team develops an individualized treatment plan. “It’s not enough to simply say ‘breast cancer’ anymore,” notes Harkness. “It’s ‘What kind?’ Because treatments we do are far more individualized for both the patient and the type of breast cancer we’re dealing with. So the first step is really understanding the imaging, the biopsy result and the subtype of cancer someone has, and then coming up with the best order and combination of treatment.
“Most breast cancers,” he continues, “need some combination of surgery, radiation, chemotherapy and hormonal therapy; some cancers need all, but not every one. The order and combination depend on the subtype and the stage.”
With new tests, says Harkness, oncologists can ascertain the tumor’s genetic makeup and, based on that, determine whether chemotherapy is likely to be effective. “We use a lot less chemo for breast cancer than we used to, but hopefully we’re giving it more to people who will actually benefit from it.” He adds that while some chemo regimens are harder to tolerate, thanks to better anti-nausea medications, the experience isn’t nearly as bad as it used to be.
Positive trends
Despite the challenges, professionals engaged in the battle against breast cancer find reasons for optimism.
For Fleeman, the recent advances in sophisticated imaging are a key factor. “We like 3D because we see better and it’s harder for the cancers to hide,” she says. “Our goal is to find and treat cancers early. With screening-detected cancer, the patient has to have less extensive surgery and less chemotherapy. When we find a cancer at Stage 1, it’s just a bump in the road.”
Wilson, the genetic counselor, cites insurance companies’ increased acceptance of genetic testing. “They used to look at it as kind of experimental, but now it’s really standard of care, because it can really make a difference financially and medically. If, through genetic testing, you can get someone the right treatment from the beginning versus failing five other treatments first, it makes a tremendous difference and impacts outcomes.”
Harkness, meanwhile, believes, “The biggest thing with breast cancer is how much research is being done. We have seen such dramatic strides in different areas of breast cancer over the last couple of decades; we are constantly refining and making advances. While nobody can know what that next thing is going to be, the trajectory of how much better we do in finding, treating and curing breast cancer today than we did even 10-15 years ago is where I find optimism.”



Before you comment
The comments section is here to provide a platform for civil dialogue on the issues we face together as a local community. Xpress is committed to offering this platform for all voices, but when the tone of the discussion gets nasty or strays off topic, we believe many people choose not to participate. Xpress editors are determined to moderate comments to ensure a constructive interchange is maintained. All comments judged not to be in keeping with the spirit of civil discourse will be removed and repeat violators will be banned. See here for our terms of service. Thank you for being part of this effort to promote respectful discussion.