A recent Tuesday afternoon at the Western North Carolina Birth Center was unusually quiet. The birthing rooms were empty. No laboring mothers paced the halls; no infants wailed. The staff arrived for work, but the mood was forlorn.
July 20 marked the close of the WNC Birth Center, the only 24/7 midwifery option in Asheville. The nonprofit provided OB-GYN services and midwifery care as an alternative to giving birth in a hospital. Nancy Koerber, the center’s executive director, announced the closure in a June website post that cited both ongoing and unforeseen challenges.
“We still are hanging on to hope,” said Koerber during a July 13 interview at the center’s waiting room for families. “But the birth center will be closing on July 20. If it is able to reemerge in some capacity, that will happen down the road.”
Since the nonprofit’s founding in 2016, Koerber estimates its team has birthed 1,032 babies, including 300 this year. But in recent weeks, its four certified nurse midwives, or CNMs, and two nurses have been coordinating with patients to transition them to other providers.
After the center’s closing, only two accredited birth centers — one in Chapel Hill, the other in Statesville — remain in North Carolina. The Asheville facility is the fifth accredited birth center to close in the state in five years, says Koerber.
Different strokes
Birth centers offer expectant mothers a middle ground between giving birth in a hospital setting and a home birth. “The medical community was willing to support having a free-standing birth center — they felt like it would meet the needs of the community who would not want to birth in the hospital,” explains Koerber. “There’s a lot of people who don’t want to birth in the hospital, for various reasons.”
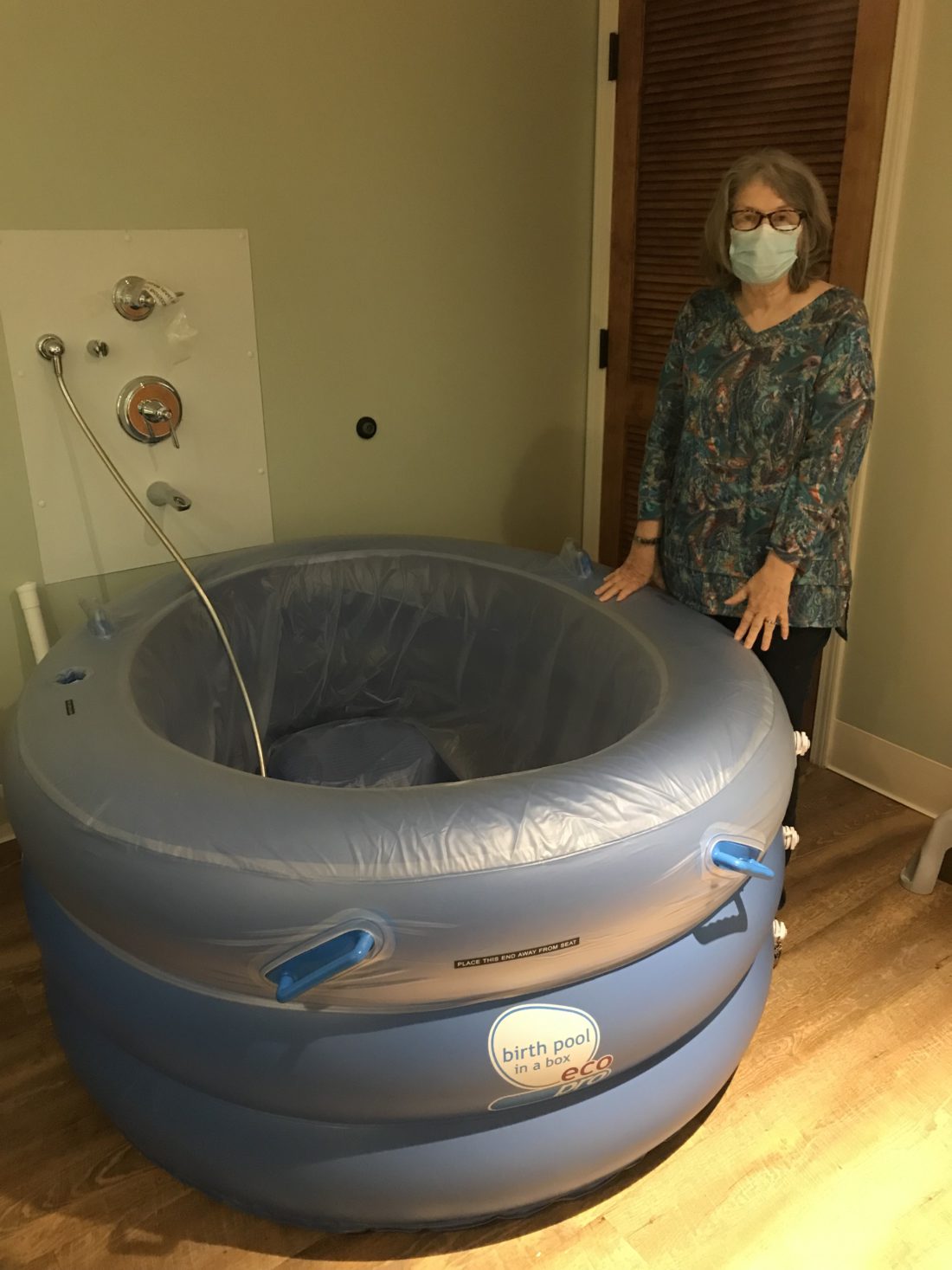
Expectant mothers may choose a birth center because the setting appears less medicalized, with an atmosphere designed to feel more homelike. For example, each room at the WNC Birth Center resembled a cozy bedroom with a queen-sized bed and piles of throw pillows atop quilts. Fertility artwork and intricate tapestries hung on the walls. Only the presence of a large blue inflatable birthing pool in the corner indicated that new life came into the world in the room.
Unlike a traditional hospital room, the rooms at the WNC Birth Center didn’t have oxygen tanks or IVs set up beside the beds. That equipment was stored in a nearby closet and taken out for use as needed.
A birth center can be a good option if the mother and child are healthy and the mother doesn’t want pain medication during labor, according to the N.C. Affiliate of the American College of Nurse Midwives. They are not advised when a mother has certain health conditions such as placenta previa, is carrying multiples, goes into early labor or plans a cesarean section.
Some women may begin to labor at a birth center but then be transferred to a hospital if they require pain medication or there are concerns about changes to the baby’s heartbeat. The WNC Birth Center’s CNMs all had medical privileges at Mission Hospital, which allowed them to accompany women to the hospital in case of an emergency.
Money woes
The nonprofit’s annual operating budget is about $1.7 million, Koerber says, adding it had “significant capital debt from the remodeling of the center” in 2016 before the facility opened.
But insurance proved the birth center’s most insurmountable difficulty. Koerber explains that private insurance providers such as Blue Cross Blue Shield of North Carolina, as well as Medicaid, generally reimburse the nonprofit at lower rates than its expenses.
Self-paid customers at WNC Birth Center were charged approximately $8,600 for labor and delivery for complete maternity services and the facility fee, Koerber says. For clients on Medicaid, accounting for about 40% of patients, the center would lose $2,000 on every birth; for those with most private insurance companies, the center typically lost $1,000 per birth.
Fifty percent of the birth center’s clients are insured by Blue Cross Blue Shield of North Carolina. Jami Sowers, a spokesperson for Blue Cross Blue Shield of North Carolina, declined to confirm reimbursement figures provided by the WNC Birth Center. “Reimbursement rates vary based on the provider and individual’s insurance plan,” she wrote in a statement to Xpress.
In response to its financial struggles, the WNC Birth Center launched a fundraising campaign in January with a $250,000 goal for operations support. Koerber expressed gratitude for the donors and the $60,000 they raised, but the total underscores that more substantial financial backing is needed if the center is to reopen.
Previous attempts to seek foundational support for the WNC Birth Center have led to dead ends. “We have sought the assistance of a number of local foundations but didn’t fit their target criteria,” Koerber explained in an email.
Call the midwife
Another challenge facing the birth center is North Carolina legislation regulating midwives, which is stricter than that in many other states. Those inhospitable regulations, Koerber says, led to difficulties in attracting staff.
Most states allow direct-entry midwives — those without a nursing degree, including certified professional midwives, or CPMs — to have licensure. But only CNMs, who have a graduate-level education in midwifery, can be licensed to attend births in North Carolina. CPMs, who are credentialed by the National American Registry of Midwives and trained to facilitate births both in and out of a hospital setting, may not legally carry out those duties.
The state also requires that CNMs have the supervision of a physician. Nineteen states require a collaborative practice agreement establishing a working relationship between a CNM and a physician. But only North Carolina, Nebraska and Georgia require a supervisory agreement from a physician in order for a CNM to practice, explains Suzanne Wertman, state government affairs consultant for the ACNM.
Under a supervisory agreement, the physician doesn’t need to be present at births, but he or she must be available for consultation if needed. “Anytime there’s a requirement for a contract with a physician, it gives that physician control of our profession,” argues Wertman.
“The required collaborative practice agreement is considered an older model,” says Dolly Byrd, director of clinical research for obstetrics at Mountain Area Health Education Center. “Other states have abandoned that and encouraged more collaboration with physician colleagues, as opposed to more hierarchical supervision.”
Pushed out
Following the closure of the WNC Birth Center, women seeking midwifery care do have other options, primarily in affiliation with area hospitals. MAHEC employs seven CNMs who each have medical staff privileges at Mission Hospital, says Byrd. Those CNMs are part of a pool with physicians to be on call for labor and delivery, she notes, and they don’t provide midwifery service overnight or on weekends.
Mission Hospital and Mission Hospital McDowell, the two hospitals operated by HCA Healthcare with a labor and delivery department, also employ CNMs. While CNMs are not available 24/7, there are OB physicians and OB nurses available.
Mission’s labor and delivery department provides expectant mothers tools that birth centers also use, like birthing tubs and birthing stools, says Mary Cascio, director for women’s services at Mission Hospital Asheville. She also notes that the only neonatal intensive care unit in the area is located at Mission Hospital Asheville. “Even the healthiest of mothers can run into a medical emergency during the birthing process, during which being in the hospital can help save that baby’s life,” she says.
Adds Nancy Lindell, spokesperson for HCA’s North Carolina division, “Mission offers the type of birthing experience that mothers want to have. However, we prioritize the health of the mother and the baby and have the emergency services available should that birthing experience not go exactly as they had hoped.”
Nevertheless, the obstetrics community is concerned by the narrowing of options for an out-of-hospital birth experience. Koerber worries about families who do not want a hospital birth or who live in obstetrical deserts where there are few options for OB-GYN care, “feeling inclined to take matters into their own hands and do what we call a free birth” — a home birth without a midwife or physician present.
“This is a community with such a rich midwifery tradition that it’s just so sad to see options reduced for women,” adds Byrd. “The birth center provided a safe option for women to have choice in their place of delivery and the type of care they received. I’m just so saddened to have that option reduced.”


Before you comment
The comments section is here to provide a platform for civil dialogue on the issues we face together as a local community. Xpress is committed to offering this platform for all voices, but when the tone of the discussion gets nasty or strays off topic, we believe many people choose not to participate. Xpress editors are determined to moderate comments to ensure a constructive interchange is maintained. All comments judged not to be in keeping with the spirit of civil discourse will be removed and repeat violators will be banned. See here for our terms of service. Thank you for being part of this effort to promote respectful discussion.