Imagine being told by doctors that, even though you are in your 20s, you have an old man’s body and must accept that you are always going to be in pain. This was the case for Adam Bradshaw, now 30. “Pain eats you up day in and day out and becomes overwhelming, and when you don’t know how to stand outside of it a little bit, it just controls you,” Bradshaw says.
What are the challenges and the options for Asheville-area patients?
“Clearly there is overprescribing of pain medication in our country, and it can go from opioids to heroin addiction,” says Bradshaw. “About every doctor I saw was glad to write me a prescription for pain meds, but I thought, ‘No, I want to try other avenues.’”
He consulted with Asheville practitioners for Chinese medicine, herbal remedies, acupuncture and psychotherapy. Bradshaw’s not alone.
According to the Centers for Disease Control and Prevention, more than 1.5 billion people worldwide suffer from chronic pain, and the rate of overdose deaths involving opioids has increased by 200 percent since 2000. In February, President Barack Obama proposed $1.1 billion in new funding to address epidemic abuse of heroin and prescription opioids.
In a July 1 Huffington Post blog, American Nurses Association President Pamela Cipriano wrote, “We must promote alternative treatments, including physical and occupational therapy, acupuncture, mindfulness and other holistic approaches, [even though] many of these alternative treatments, which a nurse might recommend for pain management, are not covered by insurance companies to the extent that drugs are, if at all.”
Will Hamilton, an Asheville psychologist, chronic pain educator and owner of Be Health AVL, says, “The problem is that 10-15 percent of the population have chronic pain, and there is a good chance they will be on medication for years.”
He points to three types of non-medication treatment: manipulative therapies (massage, physical therapy, acupuncture), movement-based approaches (like walking or gentle yoga) and stress management. “Most primary care providers are very well-trained in acute pain management, for which opiate analgesics generally work very well,” says Hamilton. “However, chronic pain management is its own subspecialty … with aspects of anesthesiology, psychiatry, neurology and physical medicine.” And managing some patients — such as those with histories of addiction — can be remarkably difficult when relying solely on medication, Hamilton says.
“Many patients feel unable to perform any activity due to their level of pain, and they often want medications that can help them function better,” he says. Under new CDC guidelines that require lower doses of medication for chronic pain patients, medical providers may not always be able to comply with patient requests for more medicine, Hamilton continues.
He hopes to address some of these challenges in an upcoming eight-week program that will focus on pacing, education and mindfulness as alternative approaches for chronic pain management (see “Chronic Pain Group” for full details). Program collaborators include Libby Hinsley, physical therapist and director of the therapeutic yoga program at the Asheville Yoga Center, and acupuncturist Lisa Sherman.
“The [program’s] group setting is important,” says Hinsley, who will lead yoga-therapy sessions. “Manual physical therapy can be helpful, but with chronic pain [patients] need to do movement for themselves.”
Hamilton also mentions pacing and breathing exercises, combined with mindfulness techniques, as program highlights. “We will look at the pain instead of reacting to it,” he says.
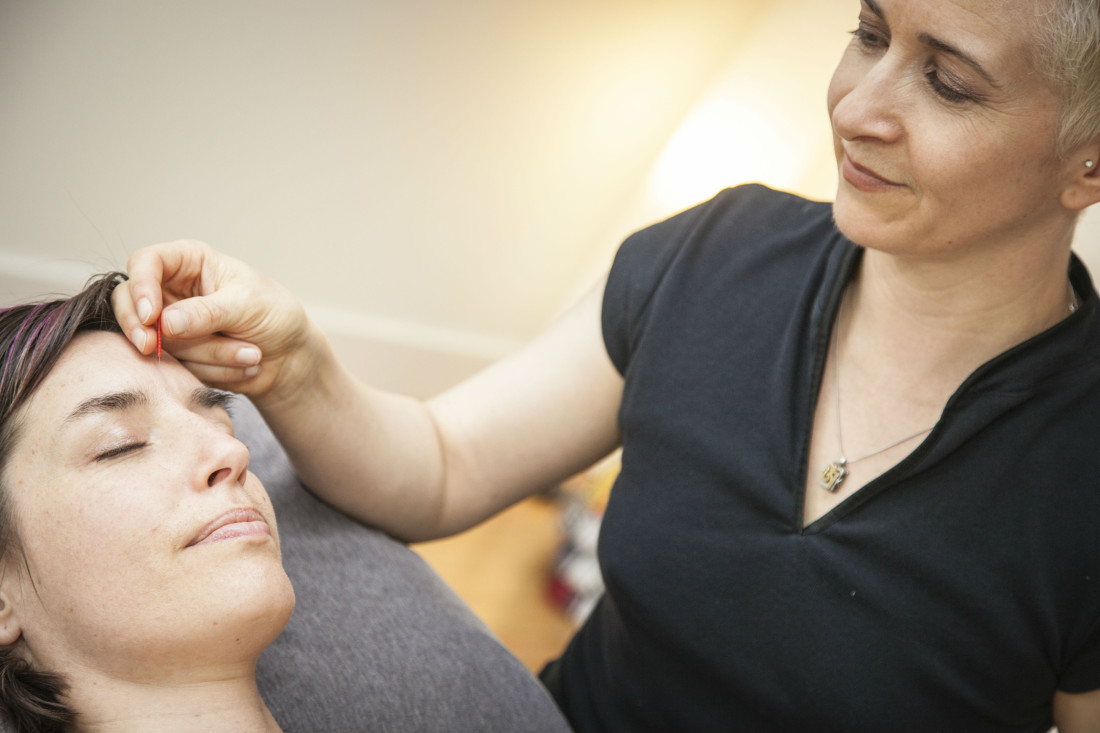
Sherman offers acupuncture in the series. “The needles can ‘hack’ the nervous system,” she says. “Putting fine needles in the ear stimulates the vagus nerve, the primary nerve of the body’s parasympathetic nervous system, and this switches on the relaxation response and switches off pain centers in the brain.”
She notes that acupuncture is now widely used in the American military and some emergency rooms as an alternative to opioid painkillers, which have negative side effects, such as addiction.
One of Sherman’s longtime patients, Sharon Gordon, says, “The funny thing is, I see how people can become attached to [medication].” She was recently prescribed oxycodone after knee surgery. “It not only relieves the pain but also gives you an energy boost, and you know when it starts wearing off,” says Gordon. “You feel like you need to take a nap.”
She has turned to massage, acupuncture and meditation to help manage chronic pain and stay off medication.
Clinical psychologist Lori Johnston works directly with patients to help them reduce their use of pain meds. “All of the research we see now is definitely pointing to the fact that integrative or combined interventions are what work best,” says Johnston, who is acting director of the Veterans Integrative Pain Management program at the Charles George VA Medical Center in Asheville.
“I bring … coping strategies and positive self-talk. [The VA] also offers acupuncture and physical therapy. We offer a lot of tools in their toolbox, not just medication.”
Cutting back on opioids is a stress factor that behavioral therapy helps to manage, says Johnston. She and her team encourage patients to identify behavioral changes by using statements such as “I am doing better because of ‘x.'” She cites a few examples, including, “I must be feeling better because I got out of the house every day this week,” or “I haven’t isolated, and I am focusing on more pleasant and positive experiences.”
Pain doesn’t have to be the controlling factor in one’s daily life, Johnston says.
Yet, many patients whose doctors reduce or eliminate their pain medications don’t understand why; they’re angry, especially those who have been on them for 20 years or more, says Johnston. A VA class about anatomy and pain conditions can help. A clinical nurse specialist leads the program, she says.
By the end of one recent class, three vets were practicing tai chi, one had joined a mindfulness-based cognitive processing group, and another veteran was finally able to go fly-fishing for the first time in years.
“They come in thinking [that] only surgeries and medications are possible and then begin opening up to these new possibilities for pain management,” says Johnston. “It is impressive when you start to see change.”
Derek Kasten, pediatric chiropractor and owner of One Love Chiropractic, says increased spinal mobility can alleviate pain. “Ninety percent of brain function comes from mobility in the spine,” he says. “If the spine moves well, it stimulates function within brain and body.”
Alignment moves the person into the parasympathetic nervous system and out of sympathetic overdrive, which exhausts the body, says Kasten. Both children and adults benefit. “Finding and removing the cause of the physical or emotional pain or releasing the interference that the stress has caused is the key, not just covering it up with a pill,” he says.
“Pain is a way the body is telling you something is not right, and we can overthink and diagnose something, like we think it could be a slipped disc or bulge, but the majority of people I see have chronic issues,” Kasten says.
“When you are in pain, you want a quick fix. You want something to break the cycle of the negative feedback loop,” he says. “Drugs … are a quick fix, but are never a long-term correction.”
Reducing pain frees up the energy that’s “going to pain and limitations” and helps the immune system, Kasten continues. “It’s amazing what the body can do,” he says.
Bradshaw agrees. “I knew I needed to listen to my body. It was trying to tell me something. The goal of these [chronic pain management] programs is to isolate it and lower the pain enough [so that] it doesn’t scream at you anymore.”
More Info
Asheville Integrated Acupuncture
Asheville VA Medical Center
Be Health AVL
Centers for Disease Control and Prevention
One Love Chiropractic
Chronic Pain Group with Be Health AVL
WHAT: This 8-week series will include one hour of gentle yoga and slow, centered movement that will be accessible on a chair or the floor. The program accepts insurance. The Asheville Yoga Center, Acupuncture Asheville and Be Health AVL are co-sponsoring the series.
WHEN: Thursdays, 5:30-8:30 p.m., starting Aug. 4
WHERE: Asheville Family Fitness, 149 New Leicester Highway


Before you comment
The comments section is here to provide a platform for civil dialogue on the issues we face together as a local community. Xpress is committed to offering this platform for all voices, but when the tone of the discussion gets nasty or strays off topic, we believe many people choose not to participate. Xpress editors are determined to moderate comments to ensure a constructive interchange is maintained. All comments judged not to be in keeping with the spirit of civil discourse will be removed and repeat violators will be banned. See here for our terms of service. Thank you for being part of this effort to promote respectful discussion.