When 5-year-old Jerrez Bowman started having trouble breathing, his mother, Ratisha Shivers, feared he might have COVID-19. Then she worried that even if he didn’t have the virus that has killed a half-million Americans in the last year, bringing him to the emergency room might expose him to it.
The Asheville resident was in luck, she says, because Mission Health recently opened an emergency department specifically for pediatric patients.
Jerrez, who has a seizure disorder, had previously been to a pediatric emergency room at Wake Forest Baptist Health in Winston-Salem. “I remember wishing we had one here,” says Shivers. “We have been to regular emergency rooms, and it definitely was not the same experience.”
During some of those visits, she remembers, they found themselves waiting near an adult who was having a mental health crisis or someone detoxifying from an addiction. “It was scary for him. I had to focus on shielding him.”
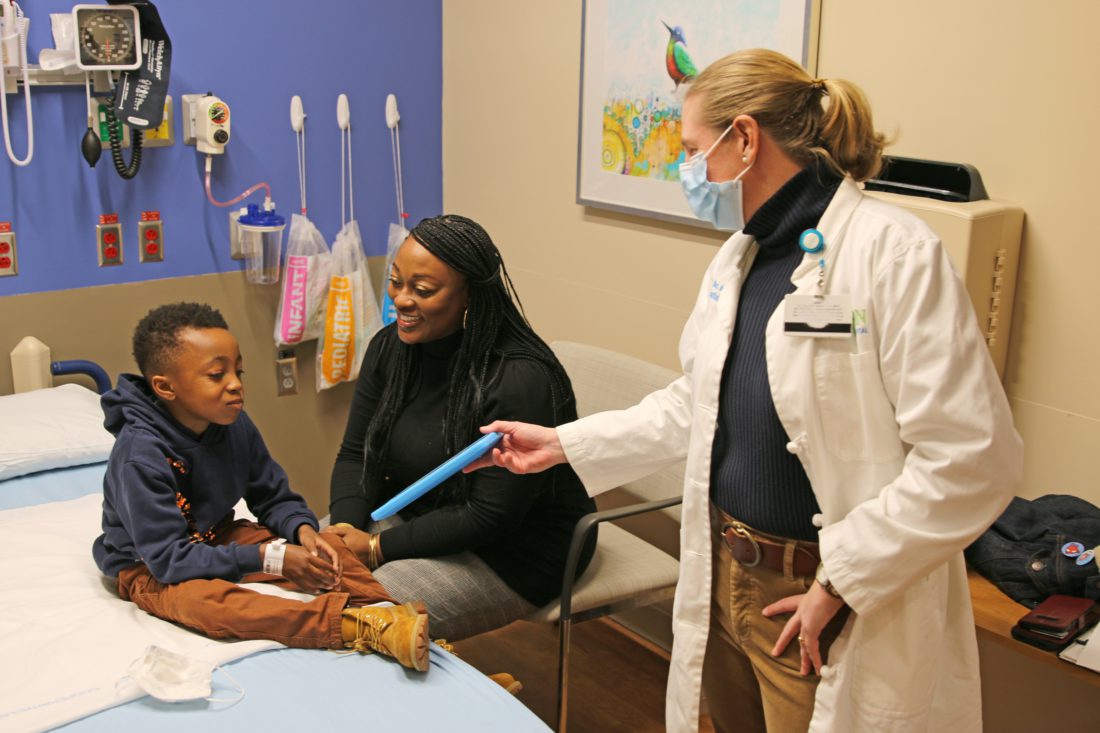
This time, though, Shivers and her son were immediately escorted to an examination room where a nurse was already waiting to greet them.
Special needs, special training
Pediatric emergency medicine became a recognized specialty in the 1980s. As academic programs were developed, specialized emergency care for children gradually became more common in hospitals. For Mission, which already had a children’s hospital, creating a designated treatment area seemed to be the logical next step, says Dr. Tyler Jones, head of the new pediatric emergency department. He trained in emergency medicine at UNC Chapel Hill and then did a fellowship in pediatric emergency medicine at WakeMed in Raleigh before coming to Mission three years ago.
As any parent who’s had to wait a half-hour in the emergency room while someone locates a pediatric blood pressure cuff can attest, having a department where appropriately scaled equipment and people who specialize in using it are readily available is a relief. Doctors who aren’t trained in how to communicate with children are more likely to miss key clues — and less likely to be able to quickly start an IV in a pint-size arm.
“This is a culmination of years of my life,” says Jones. “I had my first shift and I felt like a real pediatric emergency doctor again.”
Although Mission has had a separate children’s waiting area since the North Tower opened in 2019, Jones believes having dedicated treatment rooms can help lessen children’s trauma over needing to go to the hospital in the first place. The new unit has 12 such rooms, so patients don’t usually have to wait for one to become available.
“That was a big advantage,” says Shivers. “The doctor was there soon after, and even the discharge was really fast.” Afterward, her son asked how they could be done already when it was still daylight outside.
Regional resource
Specialized pediatric emergency departments, notes Jones, are usually found either in free-standing children’s hospitals or in bigger cities, but the arrangement works here because of the large region Mission serves.
A 2013 article in the journal Health Affairs cites problems with some pediatric emergency departments in hospitals that aren’t big enough to support them, but Jones doesn’t see that as an issue at Mission. “It’s a regional system, and all of our locations treat children,” he points out. “What we learn here can be put to use across the system. We will be a regional resource, not just for our network but for all care providers.”
Dr. Ansley Miller, medical director of inpatient pediatric services at Mission Children’s Hospital, believes the specialized environment is more calming for young patients, who may not fully understand what’s happening and why when they’re brought into a unit that primarily serves adults. “It’s a much less traumatic experience for most children,” she reports.
Jones, meanwhile, notes that having the right size equipment on hand will shorten the amount of time children have to spend in the unit, reducing their potential exposure to pathogens while helping doctors make more accurate diagnoses.
“When it comes to medicine, children are not just ‘little adults,’ they are unique!” declares a September 2020 article on the Ochsner Health blog written by a physician at the large Louisiana hospital. Medications may affect children differently, notes Jones, and their symptoms may not mirror those of an adult with the same condition.
Meanwhile, having a designated pediatric emergency department will also open up more beds for adults, who won’t be competing with children for them, says Miller.
As far as Jones is concerned, “Are there any disadvantages? Not for the children.” Having this new resource available, he concludes, “can only benefit them.”


Before you comment
The comments section is here to provide a platform for civil dialogue on the issues we face together as a local community. Xpress is committed to offering this platform for all voices, but when the tone of the discussion gets nasty or strays off topic, we believe many people choose not to participate. Xpress editors are determined to moderate comments to ensure a constructive interchange is maintained. All comments judged not to be in keeping with the spirit of civil discourse will be removed and repeat violators will be banned. See here for our terms of service. Thank you for being part of this effort to promote respectful discussion.