Caitlin Rawlins, innovation specialist for the Western North Carolina Veteran Affairs Health Care System, remembers vividly the first time that a patient at the Charles George Department of Veterans Affairs Medical Center long-term care facility used virtual reality.
“She had cognitive impairment, a history of needing stays on our inpatient psychiatric ward because of agitation or restlessness,” Rawlins explains. Then a nurse equipped the patient with a VR headset for the first time. “It was like she became a completely different person — she was wandering through this environment that was allowing her to walk through the woods, climb rocks and jump across a river.”
That virtual landscape also had deer, birds and butterflies, which brought this bed-bound patient back to times she’d enjoyed amongst the natural beauty of WNC. “Getting to be around animals and actually being able to walk — it was pretty incredible,” Rawlins continues. The patient used VR for “about an hour straight … her head was just spinning. She was so giddy.”
Charles George nurse Lynn Mennin, who works frequently with veterans who have limited physical mobility or speech, recalls giving one patient, unable to speak following a stroke, the chance to try out the computer-simulated 3D landscape of VR. Placing the headset over his eyes, she says, temporarily brought a new world into his hospital room. “He was clapping during virtual reality, pointing, and just had this big grin on his face,” Mennin explains. “He’ll look at me and [gesture that he wants the VR goggles] — like, ‘I want to try that again.’”
Over 100 VA medical centers use VR, with most starting in the past 18 months, says Rawlins. Charles George was a comparatively early adopter, acquiring its first two VR headsets in July 2018. The technology is in the early stages of being deployed in public and private health care settings worldwide. “Virtual reality in health care for clinical purposes is still in its infancy, really,” she says.
At Charles George, patients can use VR for the treatment of anxiety; stress reduction; acute and chronic pain; cognitive issues, like dementia, Alzheimer’s disease and Parkinson’s disease; and physical and occupational therapy, Rawlins explains. And the facility was the country’s first VA hospital to use the technology, in conjunction with nerve blockers, as a replacement for general anesthesia.
Another world
VR treatments at Charles George are led by nurses in its complementary integrative health care program, which provides treatments like aromatherapy, meditation and mindfulness practice and healing touch. The program has been at the hospital since 2013 to offer options for patients seeking care that complements traditional Western medicine.
Four years ago, Rawlins — then a nurse on the post-surgical ward — noted that there weren’t many non-pharmacological options to help patients manage pain after surgery. In addition to needing distractions from pain, she says, patients can often feel bored and understimulated during hospital stays.
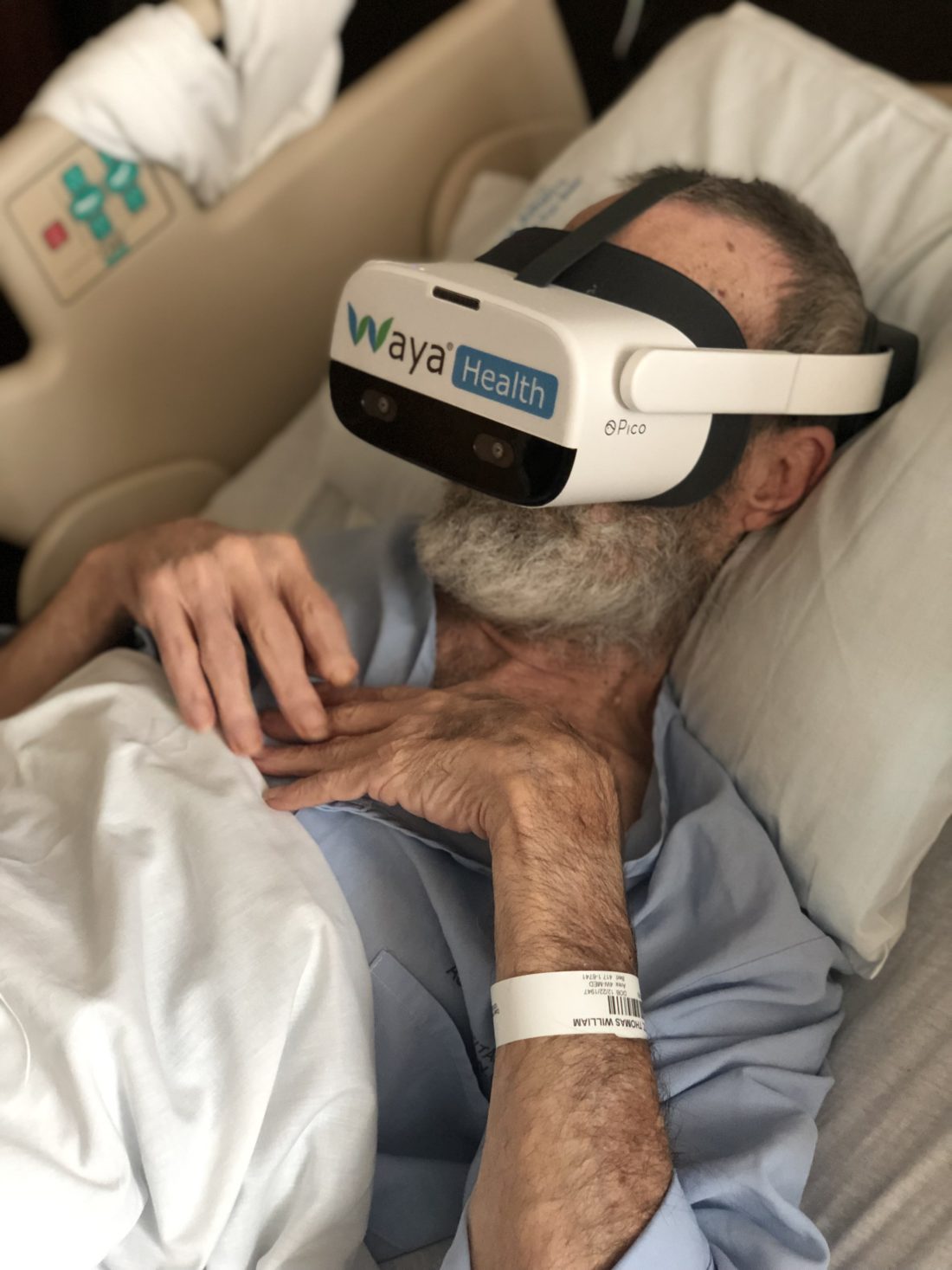
Around this time, Dr. Joe Morgan, an anesthesiologist and CEO of Boone-based Wellovate, came to speak at Charles George. The company’s physicians had created VR software called Waya Health that sought to address pain management and anxiety. Following conversations with Rawlins and others at Charles George, the hospital purchased two Waya Health headsets and began using them with patients in 2018 as part of a pilot study. Over 350 patients at the hospital have since used the technology, Rawlins says.
Clinicians are trained to recognize who isn’t a good prospect for VR, like patients with an active seizure disorder or pacemaker. (VR hardware commonly contains magnets and can interrupt the magnetically activated switch in pacemakers.) Beyond that, nurses say the training needed for both health care providers and patients to use VR is minimal.
Morgan says Charles George is an ideal laboratory for exploring clinical uses of VR because it isn’t guided by the profit motivations of private health care, which he claims can hinder innovation. “They can take bleeding edge technology like this and say, ‘Let’s see how we can use this to enable providers and help patients,’” he explains. “They don’t have to get as tied up in, ‘How do we justify this? How much money is this going to bring in?’”
Rawlins says she doesn’t have an exact figure on the expense of the VR program, as some equipment has been purchased and some donated. Additionally, the cost of software subscriptions varies by product. Charles George currently has 23 VR units, and another 27 units will be delivered at the beginning of the year. Of that total, 5 units will be donated temporarily, 18 will be permanent donations and 27 will be paid for by the facility.
According to Rawlins’ research, conducted from 2018 to 2020, 92% of 128 participants reported a distraction from their discomfort and 89% reported a reduction in stress. Ninety-six percent of participants said they enjoyed the VR experience; the top complaint among detractors was “cybersickness,” aka virtual motion sickness.
(Cybersickness is also an issue with VR used recreationally, Morgan says, recalling a floating-in-outer-space scenario that once made him feel nauseous.)
Rawlins’ findings led to her receipt of a $25,000 grant from a American Nurses Credential Center Pathway Award, which allowed her to purchase additional VR software and expand it to all Charles George inpatient care, as well as short-term rehab, long-term care and hospice at its Community Living Center. Rawlins also received a $55,000 grant from the VHA Innovators Network allowing her to lead the implementation of VR at Charles George’s outpatient facilities, as well as VA medical centers in Biloxi, Miss.; Little Rock, Ark; Memphis, Tenn.; and Reno, Nev.
Given her successes in this area, Rawlins recently became co-lead of the VHA Extended Reality Network, or XR network, coordinating innovation in the area at VAs nationwide. Extended reality is an umbrella term referring to VR in conjunction augmented reality (where the physical world is enhanced with computer-generated content) and mixed reality (a mix of the physical and digital worlds).
Growth spurt
As more VR health care products become available, Charles George has expanded its offerings. In 2020, Rawlins says, the hospital purchased products from AppliedVR and BehaVR, which primarily focus on chronic pain, and Bravemind, which focuses on prolonged exposure therapy for veterans experiencing PTSD. It also received a donation through Soldier Strong, a nonprofit providing technology to veterans, to procure REAL System, which focuses on strengthening the upper body.
The first forays into VR at Charles George required the headsets to be plugged into “high-end gaming laptops,” Morgan says, and patients needed hand-held controllers. Now, the majority of headsets are wireless, and patients with difficulty using their arms can navigate VR by sight alone.
“It has advanced to the point where you don’t even need controllers — you can literally select things in virtual reality using only your eyes,” says Rawlins. “It monitors your eye movements, and if you keep your gaze on something long enough, it’ll actually select it for you.”
Right now, Charles George’s VR setups don’t have a tactile component. But Rawlins explains that several VAs are investigating the uses of VR with haptic feedback — responsive movement — for patients. For example, she says one program is exploring VR equine therapy that allows the patient to virtually “brush” a horse.
‘Chasing dragons’
The VHA XR network, which Rawlins co-leads, and the VHA Innovation Ecosystem are collaborating with Wellovate on a second pilot study. VA medical centers in 12 locations are testing the clinical effectiveness of VR for six different uses: pain, anxiety, fall risk assessment, neurological risk assessment, palliative care and procedural use, such as in operating rooms.
Rawlins says she is particularly excited about equipping physical therapy patients with VR headsets for at-home use. “It’s like a gamified approach to physical and occupational therapy,” she says. “On their end, it looks like they’re popping balloons or chasing dragons. On the clinician’s end, they can access via the clinician portal all of the range-of-motion data related to that person’s interaction with the virtual environment.”
Chasing dragons over VR isn’t just about making at-home physical therapy exercises more fun, she continues. As a component of telehealth, VR also has the potential to reach more homebound veterans.
For now, the focus remains on finding what works. “How effective is VR at pain management, for anxiety management, for PTSD?” says Rawlins. “These are all things very much still in process. … I’m excited to see where it goes.”


Before you comment
The comments section is here to provide a platform for civil dialogue on the issues we face together as a local community. Xpress is committed to offering this platform for all voices, but when the tone of the discussion gets nasty or strays off topic, we believe many people choose not to participate. Xpress editors are determined to moderate comments to ensure a constructive interchange is maintained. All comments judged not to be in keeping with the spirit of civil discourse will be removed and repeat violators will be banned. See here for our terms of service. Thank you for being part of this effort to promote respectful discussion.