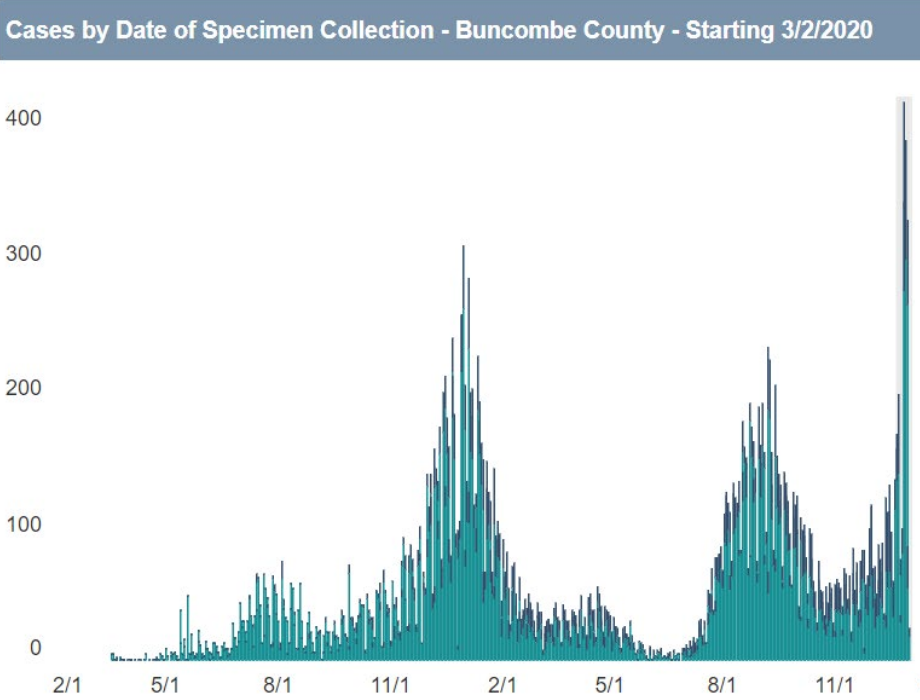
By the numbers, Buncombe County has entered uncharted territory in its encounter with the COVID-19 pandemic. Confirmed weekly cases per 100,000 residents exceeded 650 as of Jan. 3, a figure roughly 70% higher than during last winter, which Public Health Director Stacie Saunders attributed to the highly transmissible omicron variant of the coronavirus.
The county’s response, however, remains mostly unchanged. Board of Commissioners members unanimously voted Jan. 4 to extend Buncombe’s indoor mask mandate through Wednesday, Feb. 16; Saunders continued to advocate for residents to get vaccinated or receive booster shots. But aside from efforts to expand testing access, neither elected officials nor health leaders proposed new approaches for the community to weather the viral surge.
It’s unclear whether the mask requirement, reinstated Aug. 18, has significantly reduced COVID-19 transmission in Buncombe compared with surrounding counties, none of which have required masks since Gov. Roy Cooper lifted North Carolina’s statewide mandate May 14. Among those counties, only Yancey exceeded Buncombe’s confirmed per capita case rate over the past week as of Jan. 5. (Buncombe’s per capita COVID-19 death rate, roughly 174 per 100,000 residents, is lower than that of all surrounding counties except Transylvania.)
At a Jan. 5 press briefing, Saunders said she did not have data establishing the effectiveness of Buncombe’s current mask mandate. She suggested that the case rates reported by other Western North Carolina counties may be depressed due to comparatively lower levels of testing.
The extended mask requirement does not contain any language regarding enforcement, nor does it specify the type of face covering that residents should wear. Given the increased contagiousness of omicron, many health experts say cloth masks are insufficient and people should upgrade to surgical masks or N95 respirators.
Saunders agreed that those options offered more protection against omicron but said there were no plans to change the language of the county’s requirement. She said residents without access to higher-grade masks should “continue to use multilayer cloth face coverings to give that layer of protection.”
In response to reports that people have been queuing for hours at the county’s main COVID-19 testing site, located at the Harrah’s Cherokee Center – Asheville, Saunders directed questions to testing provider StarMed Healthcare. “In general, folks should expect long lines,” she said.
The county has requested testing support from both the Federal Emergency Management Agency and the N.C. Department of Health and Human Services, Saunders added, but both applications remain pending. Buncombe has also submitted an order for 5,000 at-home rapid testing kits, with plans to distribute them at community centers, fire departments, churches and other locations.
Dr. William Hathaway, Mission Health’s chief medical officer, told commissioners Jan. 4 that the “nickel lining” of omicron is that it generally appears to cause less severe disease in those infected. However, he noted, the sheer volume of cases was still likely to increase strain on the hospital system over the coming month.
“It’s not enjoyable. It’s not pleasant. Nobody enjoys doing this,” said board Chair Brownie Newman about the mask-mandate extension. “My hope is that — while the next several weeks are likely … to be really, really, rough, maybe one of the roughest periods of the pandemic — we see this peak happen soon and then quickly decline.”


Meanwhile, following the science, there continues to be no rigorous evidence in favor of cloth masks at all, and only one large study showing a 5% reduction in spread that barely rises above statistical significance for surgical masks—and those studies were run before Omicron.
Public health theater continues regardless of evidence, since it’s not founded in medicine but neurosis and fear.
Political right wing terrified white male theater continues regardless of evidence, since it’s not founded in fact but insecurity and fear.
None of this matters because this right wing, tourist friendly, overpriced, overrated, underserved and unaffordable town and it’s greedy, manipulative, apathetic, self-serving administration and the health department REFUSE to do anything to enforce the mandate. Mission refuses to mandate vaccines for their staff and the major grocer in the area, Ingles, refuses to mandate masks. Asheville is a terrifying place to be in a global pandemic.
Duh, mandates aren’t enforced so if course it will spread! smh