This summer, Kevin Mahoney decided to return to Sunrise Community for Recovery and Wellness, which he co-founded and where he will focus on educating the younger generation of peer support specialists.


This summer, Kevin Mahoney decided to return to Sunrise Community for Recovery and Wellness, which he co-founded and where he will focus on educating the younger generation of peer support specialists.

A new pilot program that started this summer helps people with opioid use disorder to initiate medication-assisted treatment in Mission’s emergency room, and then coordinates follow-up care.

The Mission Hospital Burn, Wound and Hyperbaric Center opened July 27. Services include wound care, including postsurgical and radiation wounds, surgical strategies for nonhealing wounds, hyperbaric oxygen therapy and other treatments.

MAHEC’s program is geared toward general dentists who are likely to encounter patients with a range of issues that stem from the lack of dental care. Many patients don’t see dentists because they can’t afford it.

“Focusing on access to contraception so that women can plan their family — when and if they want to have a family — is really important,” says Dr. Scott.

The Office of National Drug Control Policy has designated Buncombe, Henderson and McDowell counties as “High Intensity Drug Trafficking Areas.” More than two-thirds of Americans live in a county designated as HIDTA, according to the website.

Hathaway spoke to Xpress about having an impact on the community’s health care, how the opioid epidemic affected him as a cardiologist and his excitement over becoming a grandparent.

The reproductive landscape in America vastly changed on June 24 when the U.S. Supreme Court ruled 6-3 in Dobbs v. Jackson that abortion is not a right under the Constitution.

Childhood is romanticized as the most carefree time of one’s life. But anyone who endured bullying by classmates, or was raised with an alcoholic parent, or struggled to afford basic necessities, knows childhood has never been easy. There is widespread agreement that children’s lives have become more difficult with disruptions to education and family life […]

Buncombe County is one of the 91 counties the Office of Rural Health has designated as experiencing a behavioral health professional shortage. In fact, the 2022 departmental map designates all 16 counties of Western North Carolina as experiencing a shortage.

Mother Ocean Seafood Market is teaming with Pleb Urban Winery, offering food truck service outside the River Arts District venue. Also: PicklePalooza 2022 returns Saturday, July 23; Barn Door Ciderworks hosts its latest dinner; and more!

Buncombe County EMS has a new tool for helping an individual suffering from an opioid overdose: medication-assisted treatment, or MAT.

When Elizabeth learned that she was pregnant, she cried tears of joy. “I heard his heartbeat, and that was it,” she says. (Xpress is using her middle name to protect her privacy.) It was then that she decided to get clean. Elizabeth learned of her pregnancy while incarcerated for crimes she committed to support her […]
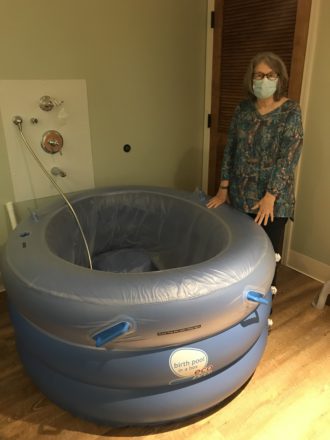
A recent Tuesday afternoon at the Western North Carolina Birth Center was unusually quiet. The birthing rooms were empty. No laboring mothers paced the halls; no infants wailed. The staff arrived for work, but the mood was forlorn. July 20 marked the close of the WNC Birth Center, the only 24/7 midwifery option in Asheville. […]

Drug abuse changed during the 13 years that Adam McIssac has been working as a drug and alcohol counselor in Asheville. At the beginning, McIssac mostly saw clients who were addicted to methamphetamine. But over time “pills,” including opioids like oxycodone (OxyContin) and hydrocodone (Vicodin), became the main drugs that his clients abused. Opioid abuse […]
As Bryan Hodge, director of rural initiatives at the Asheville-based Mountain Area Health Education Center sees it, rural communities often lack the staff and financial resources to establish and sustain residency programs.

Early data suggests monoclonal antibody therapies may reduce hospitalizations in people at high risk for severe COVID-19 complications by 70%. Limited supplies are now available in Western North Carolina.

Telehealth was already on the rise pre-pandemic, but COVID-19 has made it the new normal. Patients are ditching crowded waiting rooms en masse, opting to talk to providers from the privacy of their home.

The collaborative effort is meant to quell community fears and rumors about COVID-19 in K-12 school settings, said Buncombe County Schools Superintendent Tony Baldwin. The first report, shared Nov. 5, identified eight cases across six schools.
Based on antibody tests from six areas of the U.S., the federal Centers for Disease Control and Prevention estimates that there are an additional 10 coronavirus infections for each reported case of COVID-19. Xpress sought to determine if a similar pattern of hidden cases might hold true for the area’s coronavirus infections.

For women expecting to deliver babies this spring and summer, the coronavirus pandemic has radically reshaped much of the experience of pregnancy and birth. From online prenatal visits to limitations on the number of people who can be present at the birth to uncertainty about the medical implications of the virus for moms and babies, parents and health care providers are figuring it out as they go along.